|
Ovarian reserve refers to the quantity and quality of a woman's oocytes. The reserve declines naturally as we age, yet there is great variability in fertility rates among women of similar age.1 Identifying diminished ovarian reserve (DOR) helps predict a woman's reproductive potential and ensures we are utilizing the most appropriate interventions for our fertility patients.
Egg Quantity
Women are born with their lifetime supply of oocytes and their supply steadily declines until they reach menopause. At birth, the female ovary contains 1-2 million oocytes, by puberty the number is around 300,000 and after menopause oocyte reserves are ultimately depleted.2 Each month around 1000 follicles are recruited for maturation, though most will never reach maturity.3 In a woman's lifetime, only around 400 follicles will ever be destined for ovulation, the rest will undergo degeneration, a process called atresia. The rate of atresia is fairly steady until a woman reaches her mid-late thirties, at which time it is accelerated.4 Genetic, hormonal, and environmental influences influence the rate of degeneration.5
 Egg Quality Egg Quality
Fertility specialists define egg quality as the probability of embryo implantation. Reduced egg quality is exhibited by aneuploidy (abnormal number of chromosomes) and mitochondrial dysfunction; it is most often due to aging, but younger women can also have poor quality eggs. Risk factors include smoking, endometriosis, pelvic radiation, chemotherapy, and exposure to ovotoxic chemicals such as phthalates.6,7,8
Oxidative stress plays a central role in damaging oocyte quality. Oxidative stress results when the level of reactive oxygen species (ROS) exceeds the antioxidant defense capacity.9 Modulating ROS becomes a balancing act for oocytes, which contain the highest number of mitochondria of any cell.10 Elevated levels of ROS damage mitochondria, lipids, proteins, enzymes, and DNA, while physiological levels of ROS plays a role in oocyte maturation, ovarian steroidogenesis, and corpus luteal function.11
Assessment of Ovarian Reserve
Ovarian reserve testing is used to screen fertility patients at risk for DOR.12 The evaluation includes blood tests for follicle-stimulating hormone (FSH), estradiol, and antimüllerian hormone (AMH) as well as ultrasound imaging of the ovaries. These tests should be considered for women over 35 years of age who have been trying to conceive for six months. They should also be considered in younger women who have increased risk factors for DOR (history of smoking, endometriosis, chemotherapy or pelvic radiation) or have been trying to conceive for more than one year.
FSH and Estradiol: FSH is secreted by the anterior pituitary and stimulates the growth of ovarian follicles (Image 1); these developing follicles secrete estrogen and inhibin, leading to feedback suppression of FSH.
This baseline blood test is taken on cycle day three.
Elevated FSH may indicate DOR; values less than 10mIU/ml suggest adequate reserves and levels of 10 to 15 mIU/ml borderline.13 (Values, though, are laboratory dependent.)14
If FSH levels are normal, but estradiol levels are elevated (>80 pg/mL), this may also be indicative of DOR due to estradiol suppression of FSH.
FSH levels can vary greatly throughout cycles; a single elevated FSH value has limited reliability.15
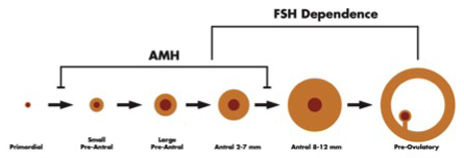
AMH: AMH is secreted by small ovarian follicles (Image 1), so blood levels of AMH reflect the size of the remaining egg supply.
AMH can be measured at any time during a woman's menstrual cycle.
Low AMH (<1.0 ng/ml) is indicative of DOR.
AMH values are stable within and between menstrual cycles.
Antral Follicle Count (AFC): The AFC is measured using transvaginal ultrasound; the antral follicles, measuring 2-10 mm in diameter, are counted and measured in both ovaries. A higher number of follicles visualized correlates with a greater ovarian reserve.
AFC is performed on cycle days 2-5.
Low AFC (< 4 to 10 follicles) suggests DOR.16
AFC is stable from cycle to cycle.
 Integrative Interventions Integrative Interventions
While the female egg supply is finite and cannot be increased (though research into ovarian stem cells is actually questioning this long held belief),17 we can improve the follicular environment to help reduce the rate of atresia and improve egg quality. Our interventions aim to reduce oxidative stress and support mitochondrial function. Three promising integrative interventions include CoQ10, DHEA, and melatonin.
Coenzyme Q10
CoQ10 plays an essential role in mitochondrial ATP synthesis and functions as an antioxidant in mitochondrial membranes. In the ovary, CoQ10 ensures adequate ATP production for developing oocytes and protects oocytes from oxidative stress. A 2015 study in Aging Cell demonstrated that CoQ10 supplementation delayed depletion of ovarian reserve, restored oocyte mitochondrial gene expression, and improved mitochondrial activity in aging mice.18 Twelve weeks of treatment with CoQ10 not only significantly increased the number of primordial follicles detected, but more pups were born to these aging female mice.19
While there are a number of animal studies demonstrating the benefit of CoQ10 on the health of oocytes, human studies are needed. Given the important role CoQ10 plays in mitochondrial function and its strong safety profile,20 CoQ10 should be considered for fertility patients with DOR. Recommended dosage is 100 mg three times daily.
DHEA
Dehydroepiandrosterone (DHEA) is a weak androgenic hormone secreted by the adrenal glands and to a lesser extent the ovaries and is converted peripherally to estradiol and testosterone. DHEA has primarily been studied in the setting of IVF as a way to increase response to ovarian stimulation, and numerous studies have demonstrated improvement in oocytes and embryo quality and yield. A 2015 Cochrane Review of 17 randomized controlled trials with a total of 1496 participants found that DHEA supplementation was associated with higher rates of live birth in IVF patients.21
Interestingly, one study set out to demonstrate the beneficial effects of DHEA supplementation on IVF patients with DOR, only to find during the 12-week supplementation period 10 of the 39 fertility patients became pregnant spontaneously, prior to their next IVF cycle.22 In the remaining patients that did proceed to IVF, pregnancy rates increased from 6.9% to 17.2% after treatment with DHEA.23
DHEA's mechanism of action on the ovary is uncertain. Proposed mechanisms include increased ovarian growth factors, decreased follicular atresia, and increased expression of FSH receptors. Supplemental DHEA has been shown to improve DOR markers; decreased FSH, increased AMH, and increased AFC have all been observed following DHEA supplementation.24
Recommended dosage of micronized DHEA is 25 mg three times daily. DHEA should not be used in patients with PCOS.
Melatonin
Melatonin is a neuroendocrine hormone secreted by the pineal gland. Melatonin is most commonly associated with sleep and circadian rhythms, but melatonin also plays an essential role in the health of oocytes and has been shown to improve both the quantity and the quality of oocytes.25
Pre-ovulatory follicular fluid contains a substantial amount of melatonin, almost three-fold the concentration found in plasma.26 The high concentrations found in follicular fluid are likely present to help counteract free radicals formed during oocyte maturation, as melatonin is a potent free radical scavenger.
Melatonin also exerts its effect on ovarian function by binding to receptor sites found on follicular granulosa cells.27 Research suggests these receptor-mediated effects may include involvement in follicular development, oocyte maturation, and luteal function.28
Recommended dosage is 1-3 mg at night before bed.
Conclusion
Diminished ovarian reserves reduce the chance of a woman becoming pregnant, so ovarian reserve tests are an important component of your patient's fertility evaluation. Since age alone has limited predictive value, diminished ovarian reserve (DOR) should be a consideration when other causes of infertility have been ruled out. Recommendations should aim to help restore mitochondrial function and reduce oxidative stress.
References .pdf
 Dr. Stacy Dunn has been involved in the health, nutrition, and fitness field for over twenty-five years. She is a naturopathic physician and acupuncturist and holds additional board certification in naturopathic oncology. Her specialties include oncology, women's health, and fertility. Dr. Dunn currently resides in Chicago and is the Director of Acupuncture for Pulling Down the Moon holistic fertility centers, www.pullingdownthemoon.com. Dr. Stacy Dunn has been involved in the health, nutrition, and fitness field for over twenty-five years. She is a naturopathic physician and acupuncturist and holds additional board certification in naturopathic oncology. Her specialties include oncology, women's health, and fertility. Dr. Dunn currently resides in Chicago and is the Director of Acupuncture for Pulling Down the Moon holistic fertility centers, www.pullingdownthemoon.com.
|
![]()
![]()
![]()
![]()









 Dr. Stacy Dunn has been involved in the health, nutrition, and fitness field for over twenty-five years. She is a naturopathic physician and acupuncturist and holds additional board certification in naturopathic oncology. Her specialties include oncology, women's health, and fertility. Dr. Dunn currently resides in Chicago and is the Director of Acupuncture for Pulling Down the Moon holistic fertility centers,
Dr. Stacy Dunn has been involved in the health, nutrition, and fitness field for over twenty-five years. She is a naturopathic physician and acupuncturist and holds additional board certification in naturopathic oncology. Her specialties include oncology, women's health, and fertility. Dr. Dunn currently resides in Chicago and is the Director of Acupuncture for Pulling Down the Moon holistic fertility centers,