Full
article: Online publication only
 Charts
linked to this page are in a .pdf format, which requires the free Adobe
Reader
(formerly Acrobat Reader).
Don't have Adobe Reader? Download it here. Charts
linked to this page are in a .pdf format, which requires the free Adobe
Reader
(formerly Acrobat Reader).
Don't have Adobe Reader? Download it here.
Introduction
The history of science has presented
some unusual twists and turns in man's
quest for knowledge. One researcher working quietly in one part of the world
may unwittingly be solving another researcher's problem in another location.
As we shall see in greater detail, government researchers and others, in an effort
to combat future bio-terrorist attacks, have unknowingly contributed greatly
to Lyme disease research. A discovery of great importance relating to a toxin
produced by the causative agent of Lyme disease, Borrelia burgdorferi,
has been linked to a similar toxin produced by the organism Clostridium
botulinum.
The
toxicity of these and other related substances is so great that bio-terrorists
have long considered using them in terrorist attacks throughout the world. Anthrax
and its spores are only one among many of such candidate organisms. For this
reason, US government scientists and others are compelled to learn as much as
possible about these highly dangerous toxins in an effort to develop antagonists
against their fatal action. It is remarkable that the research to combat possible
future bio-terrorist attacks may be applied directly to therapeutic protocols
for Lyme disease. A description of these toxins and their biological activity
is presented below, along with a listing of therapeutic substances that may be
applied in the treatment of Lyme disease.
In 1982, the agent responsible for Lyme disease was discovered by Willy Burgdorfer,
who isolated spirochetes belonging to the genus Borrelia from the mid-guts of
ticks infecting deer, other wild animals, and dogs. Spirochetes are spiral-shaped
bacteria of very early origin in the evolutionary scheme. The causative organism
was named
Borrelia burgdorferi (Bb), after its discoverer.
Since then, the number of reports of Lyme disease have increased so dramatically
that, today, Lyme disease is the
most prevalent tick-borne illness in the United States (carried by fleas, mites,
mosquitoes,
and ticks).
Lyme Disease Toxin
Because many of the symptoms of Lyme disease involve the nervous system, it
was speculated that the spirochete produced a toxin that disrupted normal nerve
function. Through the use of DNA manipulations and a database of known protein
toxin DNA sequences, a match was made with a selected Borrelia burgdorferi (Bb)
gene and
a specific toxin in the database. Protein generated from this cloned Bb gene
was
examined biochemically and found to have characteristics similar to that of botulinum,
the toxin of Clostridium botulinum, a
zinc endoproteinase.1
The toxin from Bb belongs to a family of toxic proteins known as "zinc
endoproteinases" or metalloproteases, and includes the toxin from the organism
causing tetanus as well as those from many other well-known infectious diseases.
The
structures of this family of toxins are all very similar, as determined by x-ray
crystal
analysis.2 They all contain zinc and perform the same proteolytic function, namely,
cleaving
the chemical (covalent) bond between two specific amino acids in a particular
protein
found in nerve cells.3 The substrate for this enzyme is very large, implying
that any
inhibitor of enzyme activity blocking the entry of the substrate into the active
site must
also be very large.
One reason for learning the structure of the toxin (including the active site)
is to determine the geometry of this site, the exact positions of the atoms
that bind other atoms in the substrate. Knowing the arrangement of these atoms
permits
the development
of inhibitors of the toxin, substances that compete with the normal substrate
for
active site occupancy.4
Action of Toxin
The action of botulinum (as well as the toxin
from the Lyme spirochete) is to prevent, through its action as a proteolytic
enzyme, the release of the neurotransmitter acetylcholine. Nerve endings may
be associated with other nerves or muscles (the
neuromuscular junction). To understand this mechanism in greater detail, consider
the basic principles of nerve physiology described below.
Nerve Cells
A typical nerve cell consists of a long filament or axon, the terminal end of
which
lies in close proximity to another nerve cell. The space between them is known
as the synaptic cleft (synapse). One nerve cell communicates with another through
the
release of a chemical substance known as a neurotransmitter held within small
sacs (vesicles) lying near the terminal end. An electrical pulse travels the
length of the axon
and, when it reaches the nerve cell terminal, causes the vesicles to rupture
through the presynaptic membrane and discharge the neurotransmitter into the
synaptic cleft. The neurotransmitter is bound by a protein (receptor) in the
postsynaptic membrane
of the adjoining nerve cell causing, in turn, the transmission of an electrical
pulse
down the axon of the second nerve cell. By this mechanism, nerve cells communicate
with one
another
through the action of a neurotransmitter. One such neurotransmitter is a simple
organic substance known as acetycholine. (See Chart
1.)
The structure of acetylcholine is shown by this formula:
CH3C(O)-O-CH2-CH2-N+(CH3)3
Mechanism of Neurotransmitter Release
Only recently has the mechanism of neurotransmitter
release been understood at the molecular level. The proteins responsible for
this highly detailed process
have been isolated and characterized. Some parts of the puzzle are not as yet
completely understood, for example, the process of membrane fusion. A study of
the release
of neurotransmitters from nerve endings has also revealed the mechanism of "switching," a
process by which only one nerve among several in close proximity may be separately
fired. This switching process is analogous to a similar process occurring in
computers. Our brains work in a manner, in many ways, similar to that of computers.
(See Chart 2.)
Each vesicle within a nerve ending contains only one type of neurotransmitter.
The vesicle containing a specific neurotransmitter (NT) contains on its surface
a specific protein designated VAMP (vesicle-associated membrane protein). This
protein is
a member of a family of specific proteins, differing only in the sequence of
amino
acids forming a chain extending from the protein. If the NT is designated NTA,
the
VAMP found in the membrane of the vesicle containing NTA, will always be VAMPA.
In
other words, a specific neurotransmitter is always associated in the vesicle
with a
specific type of VAMP. Finding another type of VAMP – for example, VAMPB – on
the
surface of a vesicle containing NTA will never occur. The difference between
VAMPA and VAMPB lies only in the sequence of amino acids in the peptide (protein
chain) extending
from the protein.5
During the random motion of vesicles in the region of a nerve ending, some encounter
another protein embedded in the presynaptic membrane, designated SNAP-25 (synaptosomal-associated
membrane protein). All SNAP-25 proteins belong to a family of similar proteins,
differing only in the amino acid sequences of two
peptides extending from the protein. A particular member of this family may,
for example, be designated (SNAP-25)A. If a vesicle bearing on its surface the
protein VAMPA encounters the protein (SNAP-25)A lying in the presynaptic membrane,
the three peptides (two from SNAP-25 and one from VAMP) rapidly intertwine and
automatically form a triple helix, which twists in a manner similar to a "twist-tie" used
on bread wrappers (ATP-driven). The structure of this peptide triple helix is
similar to the triple helix found in collagen (a).5
The result of the twisting action is to draw the vesicle close to the surface
of the
presynaptic membrane. When the membrane of the vesicle contacts the presynaptic
membrane, the two membranes automatically fuse, resulting in the vesicle contents
(containing NTA) emptying into the synapse. The membrane flattens out and the
VAMP/SNAP-25 proteins (the SNARE complex) are recycled.6 (See
Chart 2.)
NSF Protein
A third protein linked to the VAMP/SNAP-25 complex
is N-ethylmaleimide-sensitive factor (NSF). N-ethylmaleimide is simply a chemical
reagent used by biochemical
researchers (not a normal body metabolite), capable
of attaching acetyl groups [CH3C(O)-] to sulfhydryl groups (-SH) as found
in
the amino acid cysteine, a constituent of many proteins. The protein NSF is "sensitive" to
this reagent (binds acetyl groups when exposed to the reagent), indicating that
its surface is rich in sulfhydryl groups. This observation gives a hint about
the activity of NSF, an agent that holds together two other proteins (VAMP and
SNAP-25). Sulfhydryl groups are normally used to bind two proteins together (cross-linking)
or to bind different parts of a single protein to each other. This is accomplished
by the elimination of two hydrogens (-H) from two sulfhydryl groups (-SH) (usually
by a single atom of oxygen, thereby forming water), resulting in a disulfide
linkage (-S-S-). For this reason, NSF
is believed to function as a link between VAMP and SNAP-25, forming a single
rigid unit.5 (See Chart 1.)
Specificity of Nerve Firing
If a vesicle having VAMPA on its surface encounters a (SNAP-25)B (or any type
other than A), no intertwining of the peptides will occur, the vesicle will not
contact the presynaptic membrane and, consequently, no neurotransmitter will
be released.
The NTA, released into the synapse, almost immediately contacts a receptor (RA)
in the postsynaptic membrane capable of binding this neurotransmitter. If this
receptor is found in nerve A (see Chart 2), this nerve only is fired (i.e., develops
an action potential that travels down the axon). Any nerve ending in close proximity
not
carrying RA in its postsynaptic membrane will not be activated. If NTB is released
into the synapse,
only those nerve endings carrying RB will be activated. By synthesizing large
amounts
of vesicles containing NTA and simultaneously synthesizing an equal number of
(SNAP-
25)A, the corresponding type of nerve is activated.5
Dietary Supplements in Lyme Disease
One of the known actions of the Lyme spirochete
toxin is to diminish the release and availability of the neurotransmitter acetylcholine,
a simple organic compound (see above for chemical structure). This substance
is biosynthesized by the body
as
required in nerve activation and transmission. Supplementation by the precursors
of acetylcholine synthesis would be of value to Lyme patients since they have
a deficiency of
this substance. (See Listing 1.)
Listing 1: Dietary Supplements
Increasing Acetylcholine
Synthesis Improving Neurologic Function
- Phosphatidylcholine
(Lecithin)Acetyl-L-Carnitine
- Vitamin B5 (Pantothenic
Acid)
- Vitamin B6 (Pyridoxine)
- Vitamin C (Ascorbic Acid)
- Lysine (Amino Acid)
- S-Adenosylmethionine (SAM) (Sulfur-bound
Adenosyl Methionine)
If the inhibition
of acetylcholine release were total, Lyme patients and those suffering
from food poisoning would not
be able to
move; they would be completely
paralyzed. Since the blockage is only partial, any increase in the amount
of available neurotransmitter would benefit anyone experiencing
neurotransmitter
blockage.
For this reason, dietary supplements increasing the amount of available
acetylcholine have been shown to benefit Lyme patients.
Acetylcholine Formation
In Chart 3, we can see phopsphatidylcholine is a constituent of lecithin, a well-
known dietary supplement. Acetylcholine is simply choline to which an acetyl
group (CH3CO-) has been attached. Lecithin is the source of choline,
and acetyl-L-carnitine (ALC) is the source of the acetyl group. Carnitine is
synthesized by the body
and requires several factors, including the amino acid lysine and vitamin C (ascorbic
acid). The supplement known as SAM (S-adenosylmethionine) supplies methyl groups
(CH3-)
to lysine, forming trimethyllysine. This compound is further processed, requiring
additional vitamin C, resulting in carnitine that supplies the necessary acetyl
group.8,9
History of Lyme and Related Spirochetal Diseases
The discovery by Burgdorfer that Lyme disease
was caused by a spirochete placed it in a category of other diseases known
to be caused by spirochetes. An example of such a disease is syphilis, the
scourge
of Europe for hundreds
of years. Arsenic
and some of its compounds had been known for quite some time as a highly
successful and popular means of fatally poisoning someone (remember the King
in Shakespeare's
Hamlet). Following the discovery of the Germ Theory of Disease by Louis Pasteur
(1822–1895), it was theorized that, if arsenic was toxic enough to kill,
it may also
be effective in killing the organisms that cause disease. In the early 1900s,
the German chemist-physician Paul Ehrlich (1854–1915) developed a chemical
treatment for
syphilis. By using a "shotgun" approach of trying hundreds of compounds
in an
effort to find one that worked, Ehrlich discovered what became known as Salvarsan
or "606" after
606 compounds had been tested. Salvarsan is an organic compound of arsenic and
may be highly toxic if not properly used. For his monumental discovery, Ehrlich
was
awarded the Nobel Prize in 1908. Salvarsan may be considered the first man-made
antibiotic.26 Arsenic belongs to that column in the periodic table of chemical
elements known as the "Group V elements," which also include phosphorus,
antimony and bismuth. (See Chart 4.)
Following the success of Salvarsan as a treatment for syphilis, other compounds
of antimony and bismuth were also prepared and tried against spirochetes. Examples
of these compounds include bismuth subcitrate, bismuth subsalicylate (Pepto-Bismol),
bismuth subgallate, and many others. An example of an antimony-containing antibiotic
is Pentostam (an antimonial, antimony sodium gluconate).27,28
A biological molecule known as ATP (adenosine triphosphate) supplies energy to
biological systems through the high energy bonds found in a chain of three terminal
phosphate groups. One of the mechanisms by which arsenic exerts its toxic effect
is the substitution of phosphorus by arsenic in ATP, since both arsenic and phosphorus
lie in the same column of the periodic table of chemical elements and have similar
chemistry. (See Chart 5.)
When this substitution occurs, the molecule experiences immediate hydrolysis,
breaks down, and no longer functions as a source of energy for the cell. Both
antimony and bismuth are also found in this column of the periodic table (Group
V). 29,30 (See Chart 6.)
What may be the first case of Lyme disease was noted about 1974 in a 14-year
old boy, taken to the hospital with extreme pains in the muscles of his legs
and unable to walk. This case, coupled with other pertinent facts related to
the boy and a
highly classified US government laboratory conducting research on contagious
animal
diseases in this same area, is suggestive of a link between these two events.
The government laboratory alluded to is found on Plum Island, just north of Long
Island, NY,
and south of Lyme, Connecticut. Because of its secret nature, access to the island
was only
by ferry boat and restricted to the government workers employed there. The 14-year
old
boy lived near the ferry boat dock. Although not providing proof, these considerations
are highly indicative of a possible link between this research laboratory and
the subsequent
outbreak in 1975 of an unknown disease involving juveniles in the same area of
Lyme, Connecticut.32 A condensed form of the history of Lyme disease is shown
in Listing 2.23
Listing 2: History of Lyme Disease
1900
Effective antisyphilitic, Salvarsan, (syphilis,
a spirochete disease) discovered by Paul Ehrlich, MD.
1908
Ehrlich awarded Nobel Prize for the arsenic-containing compound to
treat syphilis.
1952/2004
Highly classified US Government animal disease research laboratory,
Plum Island, in close proximity to Lyme, CT.
1974
First Lyme symptoms, 14-year old boy, Lyme, CT.
1975
Lyme disease first recognized by Allen Steere, MD, in Lyme,
CT.
1982
The causative Lyme spirochete was discovered by Dr. Willy Burgdorfer.
1983
Borrelia burgdorferi was named after Dr. Willy Burgdorfer.
2003
American Biologics' Bradford Variable Projection Microscope (BVPM)
images of Lyme spirochete and cyst forms.
2004
Dr. Robert Bradford, through the Bradford Research Institute
(BRI), an independent research entity, funded by American Biologics,
is the developer of Bismacine,TM a chemical compound of bismuth.
This formulation has shown to be effective at the Ingles Hospital
against the spirochete and cyst forms of the Lyme organism.
© 2004 BRI
Etiology and Difficulty of Treatment
The first step in being able to
treat any disease is to learn the cause (etiology) of that disease.
Once the cause of Lyme disease was known, it seemed that a treatment
modality would soon follow and the problem would be solved. Unfortunately,
as
history has shown, this was not to be the case. As more was learned
about the causative
agent, namely, the spirochete Borrelia
burgdorferi,
it became obvious that this
organism
was unlike any that had been previously studied. It is one of
the largest of spirochetes
(0.25 x 25 µ) Spirochetes in general are difficult to treat
for several reasons: They have the ability to burrow into or
between cells
and hide,
gaining protection from the immune
system. Both Bb and Treponema
pallidum,
the causative agent for syphilis, have highly unusual outer membranes,
and the molecular architecture of these membranes
is
responsible
for their ability to cause persistent infection.
Bb also has a three-layer cell wall, helping to determine the
spiral shape of the spirochete. This distinctive cell wall resembles
those of Gram-negative bacteria,
although Bb does not stain Gram-negative but is stained by silver
stains (containing silver
nitrate). This characteristic may be related to the purported
treatment of Lyme disease
by colloidal silver.33
Another unusual structural feature is a single flagella, attached to each end
of the spirochete, running the length of the organism and surrounded by it. This
feature
is significant in relation to immune protection, since most bacterial flagella
are
highly antigenic. Still another difference in Bb structural architecture is a
clear
gel-like coating surrounding the bacteria, giving it protection from the immune
system.31 (See
Chart 7.)
The DNA of Bb is arranged in a different manner than in other
bacteria, lying along the inside of the inner membrane, and resembling
a
net just under the
skin. The bacteria replicates specific genes, inserts them into
its own cell wall and
then pinches off that part of the cell membrane, releasing it
into the surrounding medium. This fragment of the spirochete
membrane
with incorporated DNA is
known as a "bleb." It is not understood why this strange
event occurs or what advantage it gives the organism but some
studies suggest that
the function
of blebs is to bind IgM antibodies, thereby protecting the organism
from the immune system.33 Bb is one of the most immuno-suppressive infectious agent, affecting
cellular immunity, humoral immunity, and natural killer (NK) cell population.24,
25
The spirochete is typically observed in the Bradford Peripheral Blood Assessment
(BPBA) utilizing the Bradford Variable Projection Microscope (BVPM) in three
different forms.23
I. Normal spiral form
of spirochete, length of approximately 25 µ with
evenly spaced blebs along its membrane. (See Photo 1.)
Photo 1
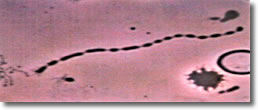
Darkfield-Phase
10,000X
II.
The elongated bleb form described above, by doubling back on itself,
forms a circle of blebs. (See Photo 2.)
Photo 2

Darkfield-Phase
10,000X
III.
The elongated form doubles back on itself, forming close-packed
multiple clusters of figure 8s (convolutions), typically observed
inside a B-cell, but
may been seen isolated. (See Photo 3.)
Photo 3
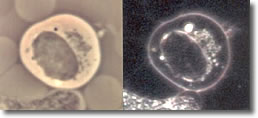
Phase
18,000X
IV.
Cyst forms developed inside a B-cell, without the clustered spiral
form of the spirochete. (See Photo 4.)
Photo 4
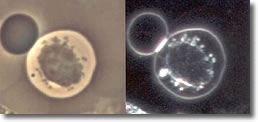
Phase-Darkfield
10,000X
V.
Cyst forms developed inside a B-cell with clustered spiral form
of spirochetesee. (See Photo 4A.)23
Photo 4A
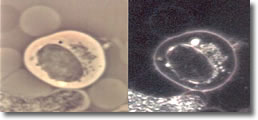
Phase-Darkfield
10,000X
VI.
Cyst forms inside a basophil. (See Photo 5.)
Photo 5
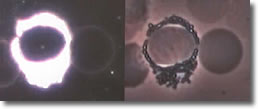
Darkfield-Phase
12,000X
VII.
Cyst forms inside an eosinophil. (See Photo 6.)
Photo 6
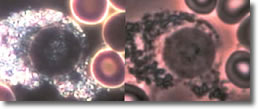
Darkfield-Phase
10,000X
VIII.
Scanning electron microscopy of blebs on spirochete membrane. (See
Photo 7.)
Photo 7
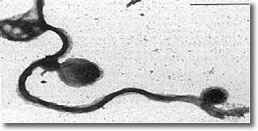
Electron Microscopy
Bb deposits cysts
inside eosinophil segments with the immune response similar to parasite
infection, resulting in increased EOC.
Photo
8 shows an infected
EOC and a normal EOC.
Photo 8
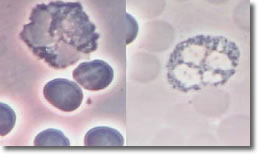
Infected Normal
Phase Phase
EOC
10,000X
Bb
deposits cysts inside basophil segments. Photo 9 shows an infected
basophil and a normal basophil.
Photo 9 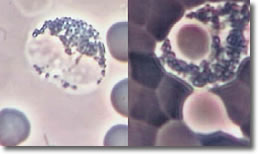
Normal Infected
Phase Darkfield
Basophil
10,000X
The
PMNs, after a finite period of time, will start to recognize
the deposited cysts in the WBCs and put their energy into
destroying the cysts. In this
process, the PMNs stop normal cytoplasmic streaming with a resultant increase
in bacteria
count. (See Photo 10.)
Photo 10 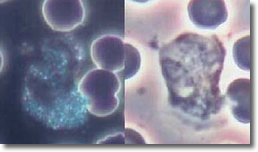
Normal Normal
Darkfield Phase
Neutrophil
10,000X
Photo
11 shows a non-infected PMN cytoplasmic streaming activity.
Photo 11 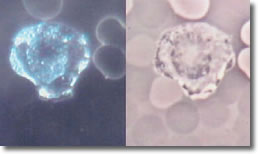
Infected Infected
Darkfield Phase
Neutrophill
10,000X
The
cell division time of Bb is very long compared to other bacteria.
A typical cell wall reproduction time for Streptococcus or Staphylococcus
is less than 20 minutes, while the total reproduction time of
Bb is from 12-24
hours.
Most antibiotics inhibit the formation of cell walls and are effective
only when the bacteria
are dividing with the formation of new cell wall. With the slow replication
time of Bb, an antibiotic would have to be present 24 hours a day for one
year and six months to be present during the cell wall reproduction period.33
There are basically two mechanisms by which Bb can survive within the host
and remain for long periods of time, unknown by the victim. Because of
these processes, a person infected by Bb can remain unsymptomatic for long
periods
of time and
then suddenly, without warning, begin to experience symptoms once again.
One of these mechanisms involves the invasion of tissues by the spirochete.
The
tip of the organism has the ability to bind to cells, spin and twirl until
it stimulates the cells own enzymes to digest a part of the membrane, finally
allowing entry. Once inside, the spirochete results in either the death
of the cell or takes up residency within. It may lie dormant for years,
protected
from both the immune system and the action of antibiotics.
Experiments have shown that, if a culture of Bb is placed under conditions
of nutrient deprivation or starvation, it senses that it cannot survive
in a metabolically active state and generates what are known as "cysts" or
small sacs attached to the organism by slender threads. Cysts contain immature
spirochetes
in a metabolically inactive form. Eventually, they break off from the parent
body and either remain lodged in tissues or enter the blood where they
are sensed as foreign antigens by eosinophils
(a type of WBC) and phagocytized. Eosinophils release granules of positively
charged basic protein that attach to the normally negative surface of cells.
They attempt to destroy the invading foreign bodies (cysts) but have little
success.33 (See Photo 12.)
Photo 12: Scanning electron microscopy
of the spirochete cyst form23 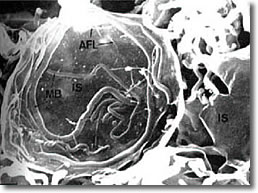
Lymphocyte
Invasion by Bb
When a spirochete attacks a B-cell, it attaches
the tip to the surface, spins and twirls until it enters, then multiplies inside
until the B-cell bursts. Some
spirochets become coated with fragments of B-cell membrane and escape detection
by the immune system by masquerading as a B-cell. Most of the antigenic proteins
in Bb (those in other bacteria mark the microorganism for destruction by the
immune system) are found on the inside of the inner membrane where they cannot
contact those WBC that detect invaders.33
Bb Surface Antigens
Experiments have shown that Bb can rather
quickly change surface antigens so that antibodies made against one strain
are effective in killing that strain, but a second strain having different
surface antigens will take up residence
in a different tissue where it escapes detection and survives. For these
reasons and others, it becomes apparent that this particular spirochete
has evolved
disguises and biological techniques to guarantee its survival and thwart
any attempts to circumvent it.33 (See Listing 3.)
Listing 3: Distinguishing Characteristics
of Borrelia burgdorfer
Internal Flagella
Glycoprotein Coat
DNA Net Arrangement
Bleb Formation
Prolonged Replication Time
Cellular Invasion Ability
|
Cyst Formation
Destruction of B-Cells
Camouflage as B-Cell
Internal Antigenic Proteins
Surface Antigen Transformation
Spiral Shape |
Nitrous Oxide (NO), A Potential Lyme Therapeutic Agent
Nitrous oxide (chemical formula
NO) is a gas, at one time commonly used as an anesthetic (laughing
gas).
In more recent times, the biochemical
activity of NO has been related to the relaxation of the small
muscle fibers in the
walls of blood vessels. They serve to either relax or constrict the
flow of blood passing through those vessels. The mechanism of NO
bioactivity
has also been learned; this involves the substance c-GMP (cyclic
guanosine monophosphate).
The amount of c-GMP at any time is regulated by the enzyme, phosphodiesterase
type 5 (PDE-5), having the capacity to destroy it. c- GMP fits into
a cavity on the surface of PDE-5, the "active site" of
this enzyme. Any other substance capable of being bound by the active
site of PDE-5 inhibits the activity of the enzyme by blocking
the entry of c-GMP,
thus allowing a greater survival of c-GMP. To summarize, any inhibitor
of PDE-5 allows an increase in the amount of available c-GMP
and consequent
relaxation of blood vessels, permitting a greater flow
of blood through those vessels.10
It has been demonstrated that NO is toxic to Borrelia burgdorferi,
the causative organism of Lyme disease.11 Therefore, any inhibitor
of PDE-5 is a potential therapeutic agent for Lyme disease. Inhibitors
of PDE-5 in common use today are the drugs sildenafil (more commonly
known as Viagra),
Levitra, and Cialis. Whether these drugs act therapeutically
against the Lyme spirochete has not been demonstrated clinically
and remains
unknown. (See Chart 8.)
Inhibitors of the Lyme Spirochete Toxin
A large amount of work is being
conducted today in an effort to uncover more inhibitors of the
Lyme spirochete toxin.
One known inhibitor of toxin activity
is the substance glycyrrhizic acid (GA), the active principle of
licorice root, used in Oriental medicine for thousands of years.12 GA
is also the active principle of the American Biologics product, Biorizin™.
The molecular structure of GA includes a steroid with large bulky
substituents.
Being a large molecule, GA is capable of binding into the active
site of the toxin, thereby blocking the normal substrate, two adjacent
amino acids
in the protein SNAP-25. (See Chart 8 and Chart
9.)
A second inhibitor of Lyme (botulinum-like) toxin is the dipeptide,
glutamylglutamate (Glu-Glu), consisting of two glutamic acids
bound together as a dipeptide.13 The tripeptide
Glu-Glu-Glu also inhibits botulinum.13 These substances
are inhibitors because of their similarity to the amino acid pair,
asparagine- phenylalanine, the normal substrate of botulinum.
Although
being bound by the toxin's active site, the toxin is unable to cleave
the Glu-Glu linkage. (See Chart 8 and Listing 4.)
Listing 4: Inhibitors of Borrelia
burgdorferi (Bb) and its Toxin
Inhibitor
Glycyrrhizic Acid (Licorice Root)
Biorizin™
Glutamylglutamate (Glu-Glu Dipeptide)
Nitrous Oxide (NO) (Arginine Stimulates Production)
Bismacine™
Chromocine™
Silver Ion
|
Inhibits
Toxin
Toxin
Bb
Bb
Bb
Bb |
© 2005 BRI
Lyme Spirochete Binds to Hostal Tissue
A specific protein (BBK32) has
been isolated from the Lyme spirochete Bb and has been shown to
bind fibronectin, the universal cellular binding agent.
This discovery may be highly significant in relation to the known
ability of Bb to become deeply imbedded and hide in most hostal
tissue.14 (See
Chart 9.)
Structure Determination of Bb Outer Surface Proteins
The structures of two outer surface
proteins (OspA and OspC) have been determined by x-ray crystal
analysis to a resolution of 2.5 A. OspA has been found to be very
different from OspC relative to the arrangement of
alpha helices and other folding of the protein.15
Structure Determination of Botulinum Complexed with SNAP-25
Botulinum, a neurotoxin produced by the
organism Clostridium botulinum is
one of the agents responsible for food poisoning. A similar toxin is
produced
by the Lyme causative organism Borrelia burgdorferi.
The detailed structure of botulinum complexed with its substrate, SNAP-25,
may lead to the development
of inhibitors of complex formation.16 (See
Chart 10.)

Major
Diseases Linked to Lyme Spirochete
Lyme Spirochete Found in the Brain
of MS Patients
The causative organism of Lyme disease, Borrelia
burgdorferi, has
been found in the brains of many victims of multiple sclerosis (MS).
The antibiotics minocycline, tinidazole, and hydroxychloroquine are
reportedly capable of destroying both the spirochetal and cyst form
of Bb. Because of this apparent correlation, it is proposed that
double-blind clinical trials be performed to confirm this finding.17
(See Listing 5.)
Listing 5: Lyme Disease Linked to Four
Major Diseases
Multiple Sclerosis, Alzheimer's, Systemic Scleroderma and Arthritis
ALZHEIMER'S
The spirochete Borrelia
burgdorferi has been found in the brain of many
Alzheimer patients. Also in the brain, antigens and genes of Bb have
been co-localized with beta-amyloid
deposits.
MULTIPLE SCLEROSIS
The spirochete Borrelia
burgdorferi (Bb) has been found in
the brain of many multiple sclerosis (MS) patients along with amyloid
deposits. MS has been linked to Lyme disease both seasonally and
by location.
SYSTEMIC SCLERODERMA
The spirochete Borrelia
burgdorferi has been found in the blood
in systemic scleroderma. Treatment with antibiotics effective against
Bb returned the skin to normal.
LYME-INDUCED ARTHRITIS
Only certain strains
of Bb are capable of causing the symptoms of arthritis.
© 2005 BRI
Lyme Spirochete Found in the Brain of Alzheimer Patients
Spirochetes found in the brain
of many Alzheimer disease (AD) patients were positively identified
as Borrelia burgdorderi,
the causative organism of Lyme disease. Borrelia antigens and
genes were also co-localized
with beta-amyloid deposits in these AD cases.18 (See
Listing 5, above.)
Lyme Spirochete Linked to Systemic Scleroderma
A patient confirmed to have systemic
scleroderma was also shown to be infected with the Lyme spirochete,
Bb. Treatment with antibiotics known
to be effective against Bb returned the skin of this patient
to normal within a few weeks.19 (See Listing 5, above.)
Lyme-Induced Arthritis Linked to Various Strains of Bb
It has been noted clinically that
some Lyme-induced arthritis patients are affected by the disease
to different degrees. A laboratory
study demonstrated that different strains of Bb were capable
of activating to various degrees a particular enzyme (matrix metalloproteinase)
found in human synoviocytes. These cells are found in the synovial
fluid of joints and form some of the substances found in this
fluid.
Matrix metalloproteinases are proteolytic enzymes capable of
degrading most of the proteins in the extracellular matrix. Different
strains
of Bb activate these proteases to varying degrees, explaining
variations seen clinically in the severity of Lyme-induced arthritis.
To date,
more than 50 strains of Bb have been identified.20 (See Chart
11 and Chart 12.)
Similarity Between DNA Sequences of Brain Tissue and Bb OspA
DNA sequences of Bb outer surface
protein A (OspA) compared with a data bank of DNA sequences of
human neural tissue yielded three
sequences that were identical. The three corresponding Bb peptides
were synthesized, and antibodies were induced against them. The
antibodies cross-reacted with human
neural tissues.
These findings imply that antibodies developed by Lyme disease
patients against OspA will also bind to their own neural tissue,
representing a form of autoimmune disease in which a person's
immune system attacks his own tissues.21 (See
Chart 13.)
Carbohydrates Consumed by Lyme Spirochete
An effort to determine which carbohydrates
Bb consumes revealed that the organism utilizes the monosaccharides
glucose, mannose and N-acetylglucosamine,
as well as the disaccharides maltose and chitobiose. A popular
treatment for arthritis includes the administration of chondroitin
sulfate and N-acetylglucosamine. If the arthritis is Lyme-induced,
N-acetylglucosamine is contraindicated.22 (See
Chart 14.)

See
Chart 15: Inhibitors of PDE-5 Increase
Nitrous Oxide, Toxic to Bb

Listing 6:
Bradford Research Institute/Ingles
Hospital Preliminary Clinical Outcome
Group I: 50 Ingles Hospital patients, Bismacine™ therapy,
100% favorable response
Group II:20 Ingles Hospital patients, Bismacine™ with Chromocine™ therapy
Reoccurrence - 3 patients (4%) in Group I
Bismacine™ with Chromocine™, our most efficacious therapy
to date.
© 2005 BRI

Listing 7: Clinical Outcome Data (Group
I) Preliminary Data
Treatment
Dates January 2004 through April 2005 (14 months)
Treatment Program BRI Bismuth Protocol
Number of Patients 55 (Male - 21 Female - 34)
Age of Patients 18 years to 76 years
Patient Response Acute Herxheimer reactions (10 days to 2 weeks)
Duration of Treatment 2 weeks to 6 weeks (in-patient)
Results
Duration of Treatment
2nd week 3
Patients - 5.6%
3rd week 19
Patients - 30.9%
4th week 20
Patients - 36.4%
5th week 10
Patients - 18.2%
6th week 5
Patients - 9.0%
© 2005 BRI

Listing 8: Clinical Outcome Data (Group
II)
Preliminary Data
Treatment Date April 2005 through May 2005
Treatment Program Bismacine™ plus Chromocine™
protocol
Number of Patients 20 (Average patients/month
- 3.9)
Male - 15
Female - 5
Age of Patients 17 years to 92 years
Patient's Response Minimal to no Herxheimer reactions
Duration of Treatment 1 to 5 weeks (in-patient)
1st week 1 Patient
5.0%
2nd week 7 Patients
35.0%
3rd week 10 Patients
50.0%
4th week 1 Patient
5.0%
5th week 1 Patient
5.0%

See
Chart 16: Clinical Outcomes
Conclusion
Bb
is one of the most immunosuppressive infectious agents known and, as
a
result,
many
secondary
infectious
agents are found along with Bb, including fungus, virus, bacteria,
and mycoplasma. Clinically, these concurrent agents
and their mechanisms are in themselves immunosuppressive and must be functionally
assessed, diagnosed, and treated in order to achieve an effective Lyme
disease program.

References
All references beginning with http:// are internet addresses.
1. Cartwright MJ, Martin SE, Donta ST. A novel neurotoxin (Bb Tox
1) of Borrelia burgdorferi. Abstracts: General Meeting of the American
Society for
Microbiology,1999:54. http://www.lyme.org/conferences/99_abstract.html
2. http://www.stormingmedia.us/18/1815/A181553.html
3. Schmidt JJ, Stafford RG. Fluorigenic substrates for the protease activities
of
botulinum neurotoxins, serotypes A, B, and F. Appl Environmental
Microbiol.
2003;69:297-303.
4. http://www.medicalnewstoday.com/index.php?newsid=8150
5. http://www.neuro.wustl.edu/neuromuscular/pathol/snare.htm
6. http://ajpcell.physiology.org/egi/content/full/285/2/C237#FIG1
7. http://www.pasteur.fr/recherche/borrelia/Borrelia_burgdorferi.html
8. Vaz FM, Wanders R. Carnitine biosynthesis in mammals. Biochem
J. 2002;361:417-29.
9. http://www.orbit6.com/cognition/neurotr1.htm
10. http://www.physiciansselect.com/L-arginine-information.htm
11. http://www2.lymenet.org/domino/nl.nsf/0/9e85f54e56d31dc5852565e30017f60f?
OpenDocument (2/6/06: Link does not work.)
12. Hayden J, Pires J, Roy S et al.. Discovery and design of novel
inhibitors of
botulinus neurotoxin A: targeted "hinge" peptide libraries.
J Appl Toxicol. 2003;23:1-7.
13. http://jmedchemdef.org/archives/CBMTSIII/cbmts3-38.pdf
14. Raibaud S, Schwarz-Linek U, Kim JH et al. Borrelia burgdorferi binds
fibronectin through a tandem beta zipper – a common mechanism.
J Biol Chem.
2005 Feb 28 (E-Published ahead of print).
15. Eicken C, Sharma V, Klabunde T et al. Crystal structure of Lyme
disease antigen outer surface protein C from Borrelia burgdorferi.
J Biol Chem. 2001; 276:10010-5.
16. Breidenbach MA, Brunger AT. Substrate recognition strategy for
botulinum
neurotoxin serotype A. Nature.
2004;432:925-9.
17. Fritzsche M., Chronic lyme borreliosis at the root of multiple
sclerosis – is
a cure with antibiotics attainable? Med Hypotheses.
2005;64:438-48.
18. Miklossy J, Khalili K, Gern L et al. Borrelia burgdorferi persists
in the brain in chronic lyme neuroborreliosis and may be associated
with Alzheimer disease. J Alzheimers Dis.
2004;6:639-49.
19. Wackernagel A, Bergmann AR, Aberer E. Acute exacerbation of systemic
scleroderma in Borrelia burgdorferi infection. J Eur Acad
Dermatol Venereol.
2005;19:93-6.
20. Singh SK, Morbach H, Nanki T et al. Differential expression of
matrix
metalloproteinases and cyclooxygenases in synovial cells exposed
to borrelia
burgdorferi. Inflamm Res. 2004;53:689-96.
21. Alaedini A, Latov N. Antibodies against OspA epitopes of borrelia
burgdorferi cross-react with neural tissue. J Neuroimmunol.
2005;159:192-5.
22. von Lackum K, Stevenson B. Carbohydrate utilization by the lyme
borreliosis spirochete, borrelia burgdorferi.
FEMS Microbiol Lett. 2005;243:173-9.
23. Bradford RW, Allen HW. Lyme Disease, Potential Plague
of the Twenty-First Century. Chula
Vista, California: Bradford Research Institute; 2004.
24. Zajkowska JM, Hermanowska-Szpakowicz T. Subpopulations of the
peripheral lymphocytes in the early clinical forms of lyme disease.
Med Sci Monit. 2000;6:278-84.
25. http://www.anapsid.org/lyme/strickerpanel.html
26. http://www.dailymirror.lk/inside/junior/020530.html
27. http://www.intox.org/databank/documents/sodstib/ukpid80.htm (2/6/06:
Link does not work.)
28. Sox TE, Olson CA. Binding and killing of bacteria by bismuth
subsalicylate. Antimicrob Agents Chemother.
1989;33:2075-82.
29. http://www.atsdr.cdc.gov/HEC/CSEM/arsenic/physiologic_effects.html
30. http://www.treedictionary.com/DICT2003/shigo/CHEM.html
31. http://www.lymenet.de/literatur/Microbiology.htm
32. Carroll MC. Lab 257: The Disturbing Story of the Government's
Secret Plum Island Germ Laboratory. New
York: William Morrow Publishing Co.; 2004.
33. Grier, T. The Complexities of Lyme Disease, from: Lyme
Disease Survival
Manual, 1997.
|

















