|
Page 1, 2, 3
Coronary heart disease (CHD) kills more than 370,000 people annually in the US.1 The standard of care for reducing this risk is to monitor a traditional lipid panel and fasting blood sugar, despite clear evidence that these two tests are inefficient. It has been demonstrated that the majority of CHD occurs in patients with normal lipid panels. The 2013 ACC/AHA (American College of Cardiology/American Heart Association) guidelines on management of cholesterol and atherosclerotic disease ignored all evidence that more in-depth testing such as LDL (low-density lipoprotein) particle number, particle size, measurements of oxidized LDL, CRP (C-reactive protein), or other easily obtainable markers hold any value despite ample evidence to the contrary.2-4
The use of fasting glucose as a measure of efficient glucose management by the body is still standard, despite evidence that it fails to detect up to 40% of active type 2 diabetics or patients with active insulin resistance.5 Given that CHD is our No. 1 killer in this country, I want to propose an approach that goes beyond our current standard to expand into the integrative model of overall health. I have already discussed primary lab options in previous articles and want to direct discussion here to treatment options and approaches.6,7
The US represents just 5% of the world population, yet we consume 50% of all the drugs made globally. If drugs truly made us healthy, then obviously we would have to be the healthiest people on the planet; but clearly this is not the case. We rank 30th in life expectancy globally and hold the world record for rates of diabetes, cardiovascular disease, and obesity. Following the 2013 ACC/AHA guidelines to offer statins to an ever-widening audience and employing polypharmacy may help modify the disease progression, but it doesn't allow us to truly reverse the course of the disease. To accomplish this, we need to attack the cause. The modern integrative care physician or practitioner has an arsenal of tools available that have been shown to be far more effective at targeting the cause of the inflammation that drives CHD.
A Brief Exploration of the History of Heart Disease
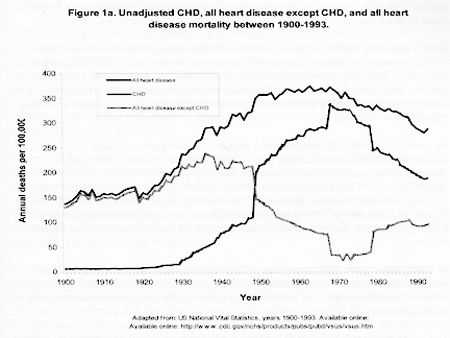
Exploring numbers from the US Centers for Disease Control (CDC), we can track the history of coronary heart disease to its origin in the 1930s.8 The occurrence of heart disease from 1900 to 1930 was nearly all structural disease, valvular issues, aneurysms, and so on. CHD was rare. In 1930, we see the first stir of CHD as processed foods became more available to the American diet. Notice the dramatic increase in CHD in 1950. What happened that year? The introduction of manufactured hydrogenated oils to the American diet. Margarine was born, and processed foods multiplied dramatically. We stopped eating food and began to eat synthetic foodlike substrates. This overlaps the advent of surgical techniques and Dr. DeBakey's solutions for structural heart disease, and soon we see death from structural heart disease plummet as CHD rises.
President Eisenhower's myocardial infarction (MI) while in office in 1955 introduced America to a new vernacular.9,10 For the first time in history, our nation was asking about the cause and condition of "heart attacks." The AMA was overrun with demands by the public for an explanation and how to avoid this new disease. It had no answer, and in frustration turned to Ancel Keys, a nutritionist and scientist of the day who had loudly proclaimed the "lipid hypothesis" as an explanation for heart disease. His theories were incorrect but gave birth to what lives today as the belief that fat causes heart disease.
Eisenhower took the advice of his physician, and removed eggs and all forms of fat from his diet and increased his use of margarine and grains. His cholesterol continued to rise and he went on to have several more MIs before he died in 1969. But as we look at Eisenhower's disease history, it is peppered with sources of inflammation, including Crohn's, arthritis, and melanoma.10 It was his high-carb inflammatory diet, inflammatory bowel disease, and stressful life that brought his ultimate demise.
Statin drugs were born in the late 1970s, and since then we have relied heavily on this growing group of drugs to corral what we thought was the cause of heart disease. By the 1990s, research had clearly shown that fat and cholesterol were not the cause of heart disease, but conveying that message to the public and to doctors is on ongoing challenge. Statins are efficacious agents in lowering the LDL, but given that this is not the cause of heart disease, the use of this approach as a sole methodology will lead to less than ideal results. The 2013 guidelines of the ACC/AHA, with 33% of members working for statin manufacturers, are not free of bias and recommended the use of a "Risk Calculator" to be employed in determining who needed statin therapy. They admitted that they had no studies to show that use of this calculator was valid, as it had not been tested in human trials.2 The Risk Calculator would dramatically increase the number of individuals who now qualify for statin use.
What is needed to return to CHD risk rates of the 1920s is not more statin use but a return to healthful lifestyle and diet. As Hippocrates once said, "Let food be thy medicine." The 2013 ACC/AHA board failed to offer any meaningful guidance here. This board offered lip service to diet and lifestyle, saying that these modalities should be used as "first-line" therapy but then fell short, as they did not offer any guidance for the application of exercise and their only dietary insight was to employ the DASH diet. The DASH diet recommends the consumption of 6 to 8 pieces of bread daily. This recommendation needs to be questioned, as the intake of a highly allergenic, high-glycemic wheat products such as bread will most assuredly drive the very inflammatory process that in fact causes atherosclerotic disease.11,12
Before we leave the topic of statin drugs, let's explore a few current controversies. Despite all of the grand statements made in defense of statins, the truth is that we need to treat 1000 people in order to stop a mere 20 to 30 heart attacks. This benefit comes at a cost both financial and physical, as statin use causes well-known side effects, leading a full 40% of all statin users to stop therapy due to complications. If we were to compile all of the well-known studies, including JUPITER, CORONA, LIPID, WOSCOPS, PROSPER, MEGA, GISSI-HF, GISSI PREV, ALLHAT, 4S, ASCOT-LLA, HPS, and AFCAPS/TEXCAPS, we would have a total of 90,056 patients. One of the concerns expressed by many is that all of these studies are funded by the very pharmaceutical companies that produce the statin drugs being tested, so there is inherent bias.
The largest statin study ever done was not funded by a statin manufacturer and needs to be included in our assessment if we are to arrive at an educated position. The Nilsson study was conducted in 2011 by a governmental agency seeking to assess the benefit of statins on reducing cardiovascular events and deaths.13 Researchers studied 4 million people over 5 years and tracked use of statin therapy and reported that they saw no evidence that statins reduced cardiovascular events or risk. This study doesn't have a pharmaceutical-funded bias and dwarfs the other studies in sheer numbers.
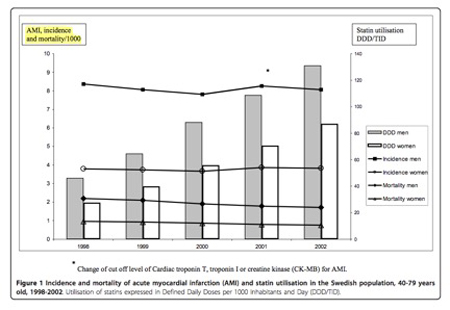
The use of statins tripled over the 5-year period, yet the number of myocardial infarctions and deaths from myocardial infarctions did not change significantly. In fact, in subgroup analysis, we saw that the occurrence rates of vascular events in men aged 50 to 59 increased 19.5% despite a 310% increase in statin use. This warrants an explanation in light of our current fascination with statin therapy.
One explanation may be the rise in diabetic disease under the influence of statins. Statins cause diabetes, and this has been shown in multiple studies.14-16 The Women's Health Initiative, after stratifying for other risk factors, determined that the occurrence rate of diabetes directly due to the use of statins was 36 new diabetic cases out of 1000 people treated.14 Other studies such as PROSPER have confirmed this effect.17 We know that 80% of deaths in diabetic patients are due to vascular disease such as CHD and cerebral vascular accidents. Does the diabetic insult caused by statin use offset their benefit, leaving us the results seen in the Nilsson study?
Studies show that CRP is twice as sensitive as LDL in predicating MI.18 CRP is more than just a marker of inflammation; it is an agent of harm, as it reduces functionality of the insulin receptor itself. Lowering CRP is critical to reversing the vascular risk and its progression. Statins may offer a modest impact here, but other tools such as hormonal balance, nutrition, nutraceuticals, and lifestyle changes offer a greater impact and certainly with less adverse risk.19-22
Exploring the Cause
The field of epigenetics has been a remarkable teacher and changed the complexion of medicine. At least 90% of chronic disease is driven by environmental exposure and not the genome.23 If we are to keep pace with the science, we need to embrace the idea that the quality of our food, water, and environment dictates disease process. Inflammation comes at us from all directions, including gut problems, poor sleep, stress, excess weight, hormones, dental factors, and all other sources that drive cytokine signaling. Food is the No. 1 element to drive all of these issues. High-glycemic, chemical-laden food drives oxidation and food allergy. A body exposed to stress and poor sleep will spike cortisol and trend toward selection of higher-glycemic foods and greater caloric intake. Stress of any kind drives weight gain, and both will combine to create rolling inflammation.
Atherosclerosis begins as a disease of the subendothelium and the vessel wall in direct response to the foods and inflammatory milieu that we create.24 Long before the first plaque appears, we can detect the inflammation lying below the endothelial surface and address it.
Page 1, 2, 3
|
![]()
![]()
![]()






