|
Today we are facing an epidemic of cardiometabolic diseases, diabetes, and obesity, both globally and nationally, which is assuming tsunami proportions. Never before have we experienced disease prevalence of this magnitude. Within 10 years, 1 in every 2 Americans will have prediabetes or diabetes.
Ninety percent of these cases will go undiagnosed. Currently, doctors are not trained to diagnose or treat these disorders early enough, and they do not have the tools that they need to deal with emerging health issues of this prevalence. They are not learning about the subtle yet complex management required by these chronic conditions in either medical school or postgraduate education.
What is needed is a systems perspective that will help providers understand the root causes of this epidemic, enabling them to prevent and address these disorders in the clinical setting. Dealing with such complex problems effectively on a day-to-day basis is going to require the insight of clinical experience – and a strong grounding in the medical literature on the positive outcomes associated with functional and lifestyle treatment of cardiometabolic conditions.
A New Perspective on Diagnosis
Finding new approaches to the management of chronic cardiometabolic illnesses will require a change in how we view and use evidence. We would suggest that to change the outcome, we must change the model.
Clinical reasoning is often grounded in heuristics (simplified models that guide evaluation and treatment at an unconscious level of awareness). The ability to utilize heuristics is a special cognitive trait, especially relevant when time and information are limited and outcomes are uncertain. This is an evolutionary breakthrough in adaptive cognition – a mindset that can be applied to benefit in the process of clinical reasoning.
The heuristic of conventional medicine achieves the stated goal of diagnosis in an expeditious manner. Clinicians apply left-brain thinking to identify the primary organ system implicated in a presenting problem and then focus the differential diagnosis within that domain. This is a computational process, without need for the type of partnership with the patient that could produce insight into the underlying causes of the patient's presenting problem.
The functional medicine heuristic, on the other hand, adds a right-brain, systems approach to clinical care that supports a carefully nurtured and protected partnership between the clinician and the patient, to illuminate the underlying mechanisms of the patient's illness(es). The FM heuristic requires an iterative, cooperative process that yields a more complete narrative story. From a thorough investigation of the antecedents, triggers, and mediators of the patient's condition, information and insight emerge to shape a deeper, more comprehensive therapeutic response.
Systems Thinking and Insight
The technical therapeutic encounter that has characterized a great deal of patient care for the last few decades can be transformed into a more effective healing partnership through a new appreciation of brain function and systems medicine. To optimize this partnership, we need to understand the process of insight as a reproducible phenomenon.
Brain research has illuminated very different functions of the left and right brain that map the neural pathways which produce insight. Solving computational questions is primarily a left-brain function. Asking a computational question triggers left-brain activity at the expense of right-brain function. (This has tremendous relevance to the interactions between doctor and patient. When a patient is interrupted with a computational question in the midst of an attempt to describe a pattern of dysfunction, the opportunity for insight may be lost.)
The left hemisphere excels at denotation – for example, storing the primary meaning of a word. It is the right hemisphere that deals with connotation, everything that gets left out of a dictionary definition. Language is so complex that the brain must process it in two different ways at the same time. As humans, we need to see both the forest and the trees.
The right hemisphere is what helps you see the forest.1,2 Much of the research into the adaptive unconscious (a.k.a. unconscious cognition) suggests that pattern recognition capacity resides in the right brain, but is not specifically localized.3,4 Solving questions that require insight generates activity that starts in the prefrontal cortex and eventually extends throughout the cortex and deeper structures, searching for possible experiential information that contributes to the emergence of a pattern.
It is the appearance of that pattern that sparks the "aha" experience in the connotative language centers of the right brain. In brief, left-brain function helps us with the denotative, computational, linear functions of life and thought, whereas the right brain provides the connotative shadings that give depth and character and color to meaning. Right-brain function is also the source of pattern recognition and insight.
Pattern Recognition and Insight
Researchers in this field have produced a robust and credible body of evidence on pattern recognition from experiments that substantiate the functions of unconscious cognition (the adaptive unconscious).5-7 Reproducible patterns of brain activity correlate with the experience of insight.8 The prefrontal cortex does not simply function as an aggregator of information. Instead, like the conductor of an orchestra, brain wave activity and energy expenditure are coordinated as if instructed by the prefrontal cortex maestro. This is known as top-down processing, since the prefrontal cortex (the top of the brain) is directly modulating the activity of other areas.
Studies show that cells in the right hemisphere have longer branches and more dendritic spines than cells in the left hemisphere. As a consequence, neurons in the right hemisphere are collecting information from a larger area of cortical space. They are less precise but better connected.
When the brain is searching for an insight, these are the cells most likely to produce it. A small fold of tissue on the surface of the right hemisphere, the anterior superior temporal gyrus (aSTG), becomes unusually active in the second before an insight. The activation is described as sudden and intense, a surge of electricity leading to a rush of blood.,9-10One of the unusual aspects of insight is not the revelation itself but what happens afterward. The adult brain is an infinite library of associations, a cacophony of competing ideas, and yet, as soon as the right association appears, we know. The new thought, which is represented by that rush of gamma waves in the right hemisphere, immediately grabs our attention. As soon as the insight happens, it becomes obvious. People often cannot believe that they did not see the connection before.11-13
Insight researchers call that "aha" experience the moment of categorical insight. The epiphany registers as a new pattern of neural activity in the prefrontal cortex. An insight is a restructuring of information – it is seeing the same old thing in a completely new way. Brain cells have actually been altered by the breakthrough. Once that restructuring occurs, you never go back.14 As Oliver Wendell Holms pointed out, "The mind, once expanded to the dimensions of larger ideas, never returns to its original size."
The Functional Medicine Matrix
These findings demonstrate the role of right-brain insight in systems thinking. Just as the development of computer technology requires both systems analysts and programmers, the future of healing is envisioned as a knowledge base that expands to incorporate systems medicine.
Functional medicine's model of comprehensive care and prevention of complex, chronic illness is grounded in both the science and the art of medicine. This model encompasses evidence on the common underlying mechanisms and pathways of disease and on effective approaches to environmental and lifestyle factors in disease. The model also incorporates the healing partnership and the search for insight in the therapeutic encounter (See Figure 1: The Functional Medicine Teaching Matrix, below).
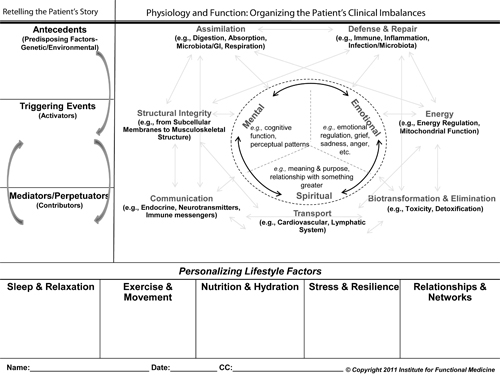
In the clinical setting, the significant answers come from a combination of the patient's experience, the provider's training and clinical experience, and the medical evidence, filtered through the clinician's insight. Clinicians are the experts on medicine, but patients are the experts when it comes to their own experience.
Our goal is to analyze, hopefully with greater and greater accuracy, the mechanisms that keep the human system functional. And when that system starts to fall apart, we want to know which mechanisms underlie that downward spiral of disease. How does the system get out of balance, start to wobble, and soon stumble toward a serious dysfunction that qualifies for an ICD-10 diagnosis?
The most important question for us as clinicians is, how far upstream can we go to identify the antecedents to susceptibility and the pathways toward (and away from) diagnosable illness? When we sit with patients, it is vital to bear in mind two primary questions: Is this person experiencing the early and unsuspected antecedents or triggers for a downstream, more serious illness? And is something happening in this patient's life that, if I fail to understand it, will result in finding the patient at the bottom of the waterfall, already in a seriously broken state?
This model is expressed in a matrix of comprehensive methodology that can be used to assess where the human system goes out of balance. The functional paradigm offers a vast range of methods for inserting the elegant tools of science into the narrative, while incorporating traditional medical treatment in a coherent way. The matrix also enfolds all aspects of the client's life.
Functional medicine informs our understanding of how the clinician triages risk, what antecedents are at play in that risk, and what mediators continue to take that patient in the wrong direction. With these tools, there is always the potential to understand steps that can be taken to change the direction, so that the patient can enjoy a healthier life. This process is based on a partnership, because as clinicians, we do not make decisions without the patient's buy-in. We want to make sure that the narrative which we are developing resonates with them. It is thrilling when the patient sees that his or her contribution is essential to a meaningful, comprehensive answer to the problem.
This is why diagnostic software programs, by themselves, have had only limited success. We know now that there is so much interplay between the belief system of the patient, his or her lifestyle, emotional life, and unique metabolism, that there are no general answers for any specific patient, regardless of the diagnosis. Consequently, when the job of the clinician is addressed only from a computational point of view, the therapy may not work as well as it needs to; patients may not even comply with the recommendations.
The Engaged Clinician
Do not ever undervalue your calling to this profession, because it is your calling that will sustain you when things get difficult. Whatever that calling is, do not lose touch with it, because there will be times when it is difficult to execute that calling. Do not give up on the hugeness of the human spirit within you and your patients, because that is what will guide you to your breakthroughs. We see these values as axiomatic for a fully engaged life as a clinician. Take solace in both the difficulties of sustaining your commitment and in the celebrations when you have stayed true to your calling, where the bigness and connections of the human spirit have been evident to you.

Notes
1. Fiore S, Schooler J. Right hemisphere contributions to creative problem solving: Converging evidence for divergent thinking. In: Beeman M, Chiarello C, eds. Right Hemisphere Language Comprehension: Perspectives from Cognitive Neuroscience. Philadelphia: Erlbaum Pub.; 1998:255-284.
2. Seger CA et al. FMRI evidence for right hemisphere involvement in processing unusual semantic relationships. Neuropsychology. 2000;14:361-369.
3. Bowden EM. New approaches to demystifying insight. Trends Cogn Sci. 2005;9(7):322-328.
4. Jung-Beeman, M. et al. Neural activity observed in people solving verbal problems with insight. PLOS Biol. 2004; 2, 500-510.
5. Chronicle EP et al. What makes an insight problem? The roles of heuristics, goal conception, and solution recoding in knowledge-lean problems. J Exp Psychol Learn Mem Cogn. 2004;30:14-27.
6. Luo J, Niki K. Function of hippocampus in 'insight' of problem solving. Hippocampus. 2003;13:316-323.
7. Siegler R. Unconscious insights. Curr Dir Psychol Sci 2000;9:79-83.
8. Bowden, op cit.
9. Bowden EM, Jung-Beeman M. Getting the right idea: semantic activation in the right hemisphere may help solve insight problems. Psychol Sci. 1998;6:435-440.
10. John Kounios J et al. The origins of insight in resting-state brain activity. Neuropsychologia. 2008;46:281-291.
11. Lehrer J. Annals of Science: the eureka hunt. New Yorker. July 28, 2008:40-45.
12. Jung-Beeman M et al. Neural activity observed in people solving verbal problems with insight. PLOS Biol. 2004;2:500-510.
13. Smith RW, Kounios J. Sudden insight: all-or-none processing revealed by speed-accuracy decomposition. J Exp Psychol Learn Mem Cogn. 1996;22:1443-1462.
14. Lehrer, op cit.

Sources
Materials from the following publications are the source of the content in this article, which was developed by Nancy Faass, MSW, MPH, director of HealthWritersGroup.com. References can be found in:
David S. Jones, MD, Laurie Hofmann, MPH, and Sheila Quinn. 21st Century Medicine: A New Model for Medical Education and Practice. Gig Harbor, WA: The Institute for Functional Medicine. 2010:1-139. Available at www.functionalmedicine.org/content_management/files/21stCentMed-FullDocument.pdf (accessed 02/18/12).
Mark Hyman, MD, and Kristi Hughes, ND. Hyman and Hughes Discuss 2012 Annual Conference. Vimeo. Available at vimeo.com/34378219. Accessed Feb. 16, 2012.
David Jones, MD, Laurie Hofmann, and Suzanne Snyder. A Clinician's Journey. Alternative Therapies in Health and Medicine. 2010 May/June:16(3);64-74.

Upcoming Conference
The Institute for Functional Medicine's 2012 Annual International Conference (May 31–June 3) focuses on "A New Era in Preventing, Managing, and Reversing Cardiovascular and Metabolic Dysfunction." A panel of distinguished faculty will offer a systems perspective on cardiometabolic disorders with practical clinical applications that can help clinicians achieve a more effective integrative approach. For additional information, see the home page of the Institute or www.functionalmedicine.org/AIC.

Nancy Faass is a writer and editor in San Francisco who has worked on more than 40 books for publishers that include Elsevier, Harper, McGraw-Hill, Mosby, New Harbinger, New World Library, North Atlantic, and others. Director of The Writers' Group, her work includes writing for the Web, and work on articles and white papers. For more information, see www.HealthWritersGroup.com.
 David S. Jones, MD, president of the Institute for Functional Medicine, oversees the development of medical education programs for the Institute and also develops partnerships and outreach. He has practiced as a family physician with emphasis in functional and integrative medicine for over 25 years and is a recognized expert in the areas of nutrition and the emerging field of lifestyle medicine. Dr. Jones is editor-in-chief of the Textbook of Functional Medicine. David S. Jones, MD, president of the Institute for Functional Medicine, oversees the development of medical education programs for the Institute and also develops partnerships and outreach. He has practiced as a family physician with emphasis in functional and integrative medicine for over 25 years and is a recognized expert in the areas of nutrition and the emerging field of lifestyle medicine. Dr. Jones is editor-in-chief of the Textbook of Functional Medicine.
 Mark Hyman, MD, chairman of the Institute for Functional Medicine, is a family physician who has dedicated his career to the whole-systems medicine approach of functional medicine. A four-time New York Times bestselling author, and author of the forthcoming book The Blood Sugar Solution, he is on the board of the Center for Mind-Body Medicine and of Memhet Oz's HealthCorps, which is tackling the obesity epidemic in America's high schools. Mark Hyman, MD, chairman of the Institute for Functional Medicine, is a family physician who has dedicated his career to the whole-systems medicine approach of functional medicine. A four-time New York Times bestselling author, and author of the forthcoming book The Blood Sugar Solution, he is on the board of the Center for Mind-Body Medicine and of Memhet Oz's HealthCorps, which is tackling the obesity epidemic in America's high schools.
Laurie Hofmann, MPH, is IFM's executive director and an advisor and consultant to several public health-care and health-education initiatives across the country.
Sheila Quinn, a freelance writer, is consulting author and editor on the Textbook of Functional Medicine and numerous other IFM publications.


|
|



![]()
![]()
![]()



 Mark Hyman, MD, chairman of the Institute for Functional Medicine, is a family physician who has dedicated his career to the whole-systems medicine approach of functional medicine. A four-time
Mark Hyman, MD, chairman of the Institute for Functional Medicine, is a family physician who has dedicated his career to the whole-systems medicine approach of functional medicine. A four-time 