Page 1, 2, 3, 4

Metabolic syndrome X (MSX) is a term that has been used to describe
a cluster of symptoms that appear together and that may increase the
risk for the development of diabetes and cardiovascular disease in
an individual. MSX has been associated with a
generalized metabolic disorder of insulin resistance and is often referred
to as the insulin resistance syndrome (IRS). The syndrome is estimated
to affect 20-25% of the adult population in the United States. Even
though many of these risk factors have been known for over eighty years,
there was not much interest in these findings until Dr. Reaven described
syndrome X in 1988 (George 2005, Reaven 1988).
Even though the term MSX has gained a great deal of popularity since
that time, there is much confusion, controversy, and doubt about its
application, particularly since no well-accepted criteria exist for
determining the metabolic syndrome in individuals. An article appearing
in USA Today by Sternberg discussed this controversy (Sternberg
2005). To date, over six organizations including the World Health Organization
(WHO), the American Heart Association (AHA), and the National Heart,
Lung, and Blood Institute (NHLBI) have their own versions of the definition
and guidelines of MSX. The most current and widely used definition
has lowered the guidelines of risk factors to near
borderline levels and suggests that the presence of any three of the
following findings warrant diagnosis of MSX:
- Central Obesity - Increased fat deposition in the abdomen. (Waist
circumference greater than 40 inches in males and 35 inches in
females)
- Dyslipidemia - Elevated triglycerides (greater than 150 mg/dl),
low HDL cholesterol (less than 40 mg/dl in men, less than 50 in females)
- Insulin Resistance - Hyperinsulinemia, hyperglycemia (fasting blood
sugar greater than 110 mg/dl)
- Elevated Blood Pressure - (greater or equal to 130/85)
Use of this definition would dramatically
increase the number of people falling into this category and consequently
being classified
as having MSX. Even Dr. Reaven, who coined the term Syndrome X stated "the
AHA and NHLBI have marched beyond the borders of scientific fact. What
the AHA did, with other groups, is to come up with a relatively capricious
diagnostic category to focus on people who are at risk of coronary
heart disease." The American Diabetes Association and European
Association for the Study of Diabetes asserted "too much critically
important information is missing" to justify the use of the syndrome
as a measure of cardiovascular and diabetes risk. Sternberg noted that
the debate has left many questions, such as when does a diagnosis genuinely
describe an illness and when does it simply give pharmaceutical companies
a bigger market?
Current Treatments for MSX
Current treatment of individuals with MSX includes weight management,
exercise, and drug therapies aimed at reducing specific metabolic
risk factors. Drug therapies include anti-hypertensive medications
for blood pressure control, statin drugs for abnormal lipoprotein
profiles, and drugs to help improve insulin sensitivity. Some of
the drug therapies have limitations and potential high risks associated
with their prolonged use. For example, statins and fibrates can
prevent lowering of HDL cholesterol but may induce severe myopathy.
Thiazides and B-blockers used for blood pressure control can exacerbate
insulin resistance. Even though metformin and thiazolidinediones
may
improve insulin sensitivity, it is unknown if they actually reduce
cardiovascular disease risk while still contributing to toxic side
effects. Even with treatment, in the long term, the metabolic syndrome
is often resistant to these therapies (Shulman et al. 2005). Improving
risk prediction of cardiovascular heart disease, an initial goal for
determining MSX, has been disappointing to say the least (Kohli, P
et al. 2006).
Factors Contributing to MSX
There are many underlying factors thought be involved in the development
of MSX, including genetic and lifestyle factors and neuroendocrine,
metabolic, and immunological imbalances as well as emotional status.
There is evidence that nutrient
imbalances are also involved, yet little information is available on
the nutritional status of individuals diagnosed with MSX. Since genetics,
lifestyle, neuroendocrine, and immunological factors contribute to
nutritional and metabolic imbalances and could be affected through
nutritional therapy, it would be reasonable to assume that MSX
could be significantly impacted by individualized nutritional therapy.
Importance of Nutrition
The need for nutritional assessment and counseling has never been more pressing
than it is today due to the epidemic of chronic disease such as obesity,
diabetes, and hypertension. It is estimated that 300,000 to 800,000 deaths
per year are the result of
nutrition-related disease. National nutritional policies and recommendations
are based largely on preventing short-term deficiencies conditions such as
scurvy, beriberi, rickets, goiter, etc. However, long-term nutritional deficiencies
and imbalances lead to major chronic disease that may take years to manifest.
Nutritional requirements needed to
prevent inadequate long-term intake are much higher than those required for
short-term deficiencies and are most often overlooked. Heaney stated that "recommendations
based solely on preventing the index diseases are no longer biologically defensible" (Heaney
2003). However, most patients who suffer from chronic disease and also have
long-term nutritional deficiency conditions receive little if any nutritional
counseling. The estimated time spent on nutritional counseling by doctors to
their patients averaged less than one minute on the subject. A report by Simopoulos
discusses the genetic variation and individuality of nutritional requirements
and stated, "The interaction of certain nutrients with genetically determined
biochemical and metabolic factors suggest different requirements for individuals,
which raises questions about the use of universal dietary recommendations for
a population" (Simopoulos 1995). It is well-known that nutritional deficiencies
as well as imbalances between nutrients develop long before signs and symptoms
of nutrition-related disease manifest. Also, evidence from the above studies
supports the view that nutritional needs should be based upon three individual
requirements rather than broad, nonspecific recommendations for a population
as a whole. This is particularly true for recommendations being made for individuals
with MSX as well as other disease conditions.
Nutritional Assessment Through Hair Tissue Mineral Analysis (HTMA)
Mammalian hair contains minerals and other substances incorporated into the
follicle during its development and locked in as the hair shaft grows from
the scalp. Incorporation of minerals into the hair is influenced by several
factors. These factors
include diet, environmental exposures, metabolic activity, disease processes,
drugs, neurological activity, endocrine activity, physiological needs, stress,
immune function, genetics, and even emotions (Watts 2005,1990, 1991, 1993,
1989, 1994, 1999, 1990). Any one or a combination of these influences will
affect nutritional status that may be reflected in HTMA studies, revealing
patterns that can be readily recognized and
associated with a number of metabolic events and health conditions. (Watts
1989, 1995, 2005)
HTMA has become a significant research tool in numerous fields of study including,
environmental, epidemiological, archeological, forensic, biochemical, and nutritional
fields (Batzevich 1995, Lal et al. 1987, Srikumar et al.1992, Pallholz et al.
2005, Nowak et al. 1998). For several decades, the US Environmental Protection
Agency
(EPA) has recognized data from HTMA studies as reliable. Human hair
is considered a meaningful and representative tissue when properly collected
and analyzed for several nutritional elements and heavy metals (EPA 1979).
HTMA is well-accepted as a heavy metal screen, but its acceptance and utilization
as a nutritional and metabolic screening tool has been criticized. Criticism
of HTMA as a viable nutritional screening tool is based upon a limited number
of studies (three), compared to the thousands of studies documenting its efficacy.
To date, there have been only a few published papers that criticize HTMA. These
studies have been small, inadequate, and flawed evaluations by individuals
with little or no experience in the field and can only be considered as evaluations
of inter-laboratory agreement. These criticisms have been addressed by several
of the laboratories performing HTMA testing as well as by myself (Watts 1999,
2000, 2001). Ultimately, these studies simply show that there is some variation
in measured results among laboratories performing HTMA. Variations can be expected
with any test between laboratories using different procedures and analytical
instrumentation.
Laboratories performing the HTMA test today have considerable experience and
expertise in this industry. Most have been in existence for more than 20 years.
They have invested considerable time and expense toward research, highly skilled
professional support staff, and the latest laboratory instruments available
for routine elemental analysis. Therefore, one can be assured that laboratory
procedures are at their finest, providing accurate, reliable test results from
hair specimens that have been properly collected according to established protocol
(Watts 2000).
Understanding HTMA
Mineral concentrations in hair are unique, and understanding the results of
HTMA is important for it to be useful in a clinical setting. Minerals are
incorporated into the hair as a result of relatively long-term metabolic
activity and are therefore more stable compared to minerals circulating in
the blood. Blood minerals, although maintained within normal homeostatic
ranges, can rapidly change as a result of short-term metabolic activity.
Mineral levels can also change in the blood over a short period of time through
consumption of food, exertion of energy, and even by modifying breathing
patterns. Also, since the blood is the mode of transport for minerals entering
or exiting the body and provides transportation of minerals that are redistributed
throughout the body, it is seldom that mineral concentrations found in the
hair will match concentrations found in circulation, except in certain circumstances
such as extreme deficiency or toxic states.
Mineral concentrations found in various organs fluctuate due to many factors,
therefore it would not be reasonable to expect hair mineral concentrations
to match organ concentration. The same is true for blood minerals verses organ
mineral concentrations. Mineral concentrations found in human hair reveal individual
mineral levels, providing an assessment of the interrelationship between nutrient
minerals and heavy metals. HTMA also provides a view into the synergistic and
antagonistic relationships between minerals. As an example, the minerals calcium
and phosphorus are synergistic in that they work together in the proper balance
for building normal bone. However, these two minerals are also antagonistic
to each other, and too much of one can cause a deficiency or increased requirement
of the other. The ideal or optimum calcium/phosphorus ratio established by
Trace Elements, Inc. (TEI) is 2.63:1. A marked elevation of calcium relative
to phosphorus would indicate an increase in phosphorus requirements, even if
the phosphorus level is within the normal range. If this ratio becomes too
low, a relative phosphorus excess would exist, thereby creating an increased
requirement for calcium and calcium cofactors such as vitamin D.
Hair Tissue Mineral Analysis (HTMA) Patterns as a Metabolic Indicator
Mineral interrelationships found in HTMA studies reveal recognizable patterns
that can be associated with individual metabolic characteristics and various
disease processes (Watts 1991). These patterns are derived from the calculated
comparison between significant macro and micro-element findings. These calculations
reveal significant mineral ratios that can be used to evaluate an individual's
nutritional mineral status and metabolic characteristics.
TEI recognizes two major metabolic categories from HTMA patterns. These categories
are termed Slow Metabolic Types (parasympathetic dominance) and Fast Metabolic
Types (sympathetic dominance). A total of eight types are recognized and include
Slow metabolic types 1-4 and Fast metabolic types 1-4.
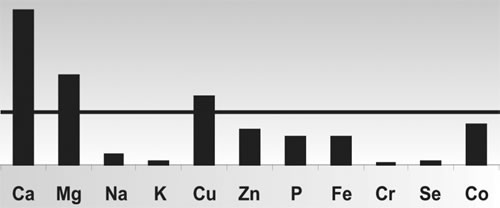
In Figure 1, we can see the mineral characteristics of the Slow Metabolic Type
1. Calcium is elevated relative to phosphorus, and calcium and magnesium are
higher than sodium and potassium.
Figure 1
Parasympathetic Mineral Pattern
Page 1, 2, 3, 4
|



![]()
![]()


