Page 1, 2, 3
KPU and Methylation
In Klinghardt's work, if a patient has KPU, treating the KPU condition first is a foundational intervention before pursuing more specific methylation support. Specific enzyme blockages are discussed earlier in this article.
In people with cancer and active EBV infection, EBV triggers a hypermethylation inside the cancer cells that may accelerate cancer cell growth. If methylation support is introduced based on genetic SNPs or other lab testing but the patient has an untreated, active EBV infection (such as is common in chronic fatigue syndrome, Lyme disease, and other related conditions) or an EBV-related cancer such as throat, stomach, breast, prostate, or Hodgkin lymphoma, supporting methylation may lead the patient to an increased risk of cancer or accelerated rate of cancer growth.
This potential makes treating KPU first even more important as balancing the zinc and B6-dependent enzymes indirectly without the addition of methyl groups is generally a safer way to restore healthy methylation on all fronts as opposed to directly supporting methylation with methyl donors.
When people begin to explore methylation, KPU should always be evaluated and addressed first. Several enzymes in or adjacent to the methylation cycle use the heme molecule which utilize zinc and vitamin B6 as primary building blocks. By supporting KPU, the methylation cycle works more smoothly, both in its ability to methylate and demethylate, and at a lower risk to the patient.
KPU and Heavy Metal Toxicity
When KPU is present and zinc and vitamin B6 are depleted, the detoxification pathways are overwhelmed and ineffective as the heme molecule is an integral part of many detoxification enzymes. Both zinc and vitamin B6 deficiencies, which are important cofactors in the methylation cycle, reduce levels of glutathione in the body. Glutathione is important for the detoxification of heavy metals and other toxins.
Replacing missing zinc and vitamin B6 increases glutathione. This, in turn, increases the rate of detoxification of heavy metals and other body burdening toxins. Once KPU treatment is introduced with zinc and B6, reducing the metal burden no longer requires heroic measures.
However, it is also the case that incorporating the KPU protocol will liberate additional heavy metals within the body. This aspect of the KPU protocol is discussed later in this article and is important for the practitioner to understand before beginning to treat patients for the condition as additional detoxification support is generally needed. This protocol is intended to be done only with the guidance of a knowledgeable practitioner.
KPU and Porphyrin Disorders
There is a group of disorders related to pyroluria called porphyrias. KPU is one of a group of conditions known as porphyrin diseases. In 100% of porphyrin diseases, the HPL compound is found in the urine.
Porphyrin testing is readily available and is a reliable tool. Klinghardt prefers to send a urine sample to Laboratorie Philippe Auguste (http://labbio.net) in France for testing. Other options are also available in the US, such as through Genova Diagnostics, Doctor's Data, and Great Plains Laboratory.
 In the US, pyroluria and porphyria are viewed as separate conditions. However, in collaboration with the Dutch lab KEAC, it has been established that everyone with elevated porphyrins has pyroluria. When pyroluria is addressed, the porphyrins go down. In the US, pyroluria and porphyria are viewed as separate conditions. However, in collaboration with the Dutch lab KEAC, it has been established that everyone with elevated porphyrins has pyroluria. When pyroluria is addressed, the porphyrins go down.
In porphyrin testing, uroporphyrin is an indicator for aluminum, coproporphyrin for lead, and precoproporphyrin for mercury. Klinghardt has not seen a case with elevated porphyrins that did not have KPU, and when the KPU was corrected, aluminum, lead, and mercury are excreted from the body, and the porphyrins go down.
This is, in part, due to the fact that when the body has been deficient in zinc for a long period of time, it may retain heavy metals much more readily. When zinc is missing from the body, it is replaced in our bones with lead. If zinc is supplemented, lead is expelled. Secondly, the enzymes needed to detoxify these metals are heme-dependent enzymes, and these metals accumulate when heme synthesis is abnormal.
Klinghardt notes that discussions on the topic of porphyria are much more widely accepted than those on pyroluria. In his experience, he finds that almost all of his patients have elevated porphyrins, and that pyroluria is the deeper core issue.
KPU and Histamine
When a KPU patient is having a good day, low histamine levels are observed; on a bad day, higher histamine levels are observed. It is the relative elevation of histamine in response to foods, inhalants, allergens, emotional stressors, and electrosmog that is problematic and causes the allergic phenomena, not the absolute histamine level. When histamine levels rise from a low level to a moderate level, the reactions are often severe.
When exploring histamine levels in a KPU patient at a time when they are experiencing hives or asthma, the histamine levels are elevated, but not to levels that would create a problem for others. The relative rise in histamine, however, in KPU patients is experienced in a far more significant way.
Klinghardt has worked with biochemists in Germany that are beginning to link KPU with mastocytosis or mast cell activation syndrome (MCAS). They have observed that KPU treatment repairs the heme molecule, which notably stabilizes the mast cells and lowers the response to these relative rises in histamine.
KPU and Multiple Sclerosis
Klinghardt has treated many patients with multiple sclerosis. The MS patients that he has tested have been highly positive for KPU. Over time, he has concluded that KPU is a frequent cofactor in MS. He has found that patients with MS respond favorably to KPU treatment.
In patients with KPU, absolute histamine levels are almost always low. The treatment for MS patients with KPU may include histamine in addition to the KPU protocol outlined in this article. Treatment with histamine may be either with oral or transdermal products. Prokarin is a transdermal patch which delivers histamine and has been used by some practitioners in the treatment of MS.
 |
 |
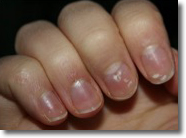
Patient with Leukodynia
before KPU treatment |
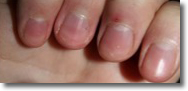
Same patient after 3 months
on KPU treatment |
Evaluation and Testing
Klinghardt recommends that people start with the HPU Questionnaire (http://www.hputest.nl/evraag.htm). Once the questionnaire is completed, a score is calculated to provide a probability that a person may have KPU. If the score is 10-14, Klinghardt will often recommend proceeding with treatment without the need for confirmatory testing as the treatment itself is generally well-tolerated. If the score is 0-9, he may suggest testing for the condition using additional lab work.
Pyrroles are impacted by light, temperature, oxygen, and time; and they readily break down. Once they begin to break down, the likelihood of detection is significantly lowered. Ideally, testing would be performed within eight hours after the collection, though this is not practical and rarely possible.
Within the United States, two of the available labs for testing include the following:
- DHA Laboratory (https://www.pyroluriatesting.com) uses a frozen one-time collection at a cost of $80. They recommend the collection be the second urination of the day. They suggest avoiding all supplements, vitamins, and minerals for 12-24 hours prior to the specimen collection. The lab is testing for hydroxyhemopyrrolin-2-one (HPL).
- Health Diagnostics and Research Institute (http://www.hdri-usa.com) charges $140 for a 24-hour collection and $90 for a random collection. HDRI suggests stopping zinc and B6 as well as antidepressant medications for 48 hours prior to the collection. They suggest not smoking or consuming caffeine for 24 hours prior. While there is no additional cost for testing the hydroxyhemopyrrolin-2-one (HPL) compound, this must be specifically ordered on the requisition form as it is not part of their KPU assay by default. If you do not specify HPL as an add-on, you will get kryptopyrrole (2,4 dimethyl-3-ethyl pyrrole) only.
In Europe, Klinghardt uses the Dutch Lab KEAC (http://hputest.nl) for HPU testing. The lab is guided by microbiologist Dr. John Kamsteeg, a world leader in HPU. The results of HPU testing with this lab align closely with the percentages of patients with chronic Lyme and other conditions that Klinghardt identifies with the HPU condition.
In Australia, KPU testing is available through SAFE Analytical Laboratories (http://safelabs.com.au) and Applied Analytical Laboratories Pty Ltd (http://www.apanlabs.com).
Each lab has their own very specific instructions for performing the test. This includes information such as shielding the specimen from light as well as how to handle and ship the specimen. It is important that the recommendations be closely followed to optimize the sensitivity of the test result.
To further maximize the sensitivity of testing, it may be best for the patient to be under stress at the time the test is being performed as HPL excretion is known to increase during times of stress.
In some circumstances, however, patients may still test negative even when the condition is suspected. In those cases, it may be best to repeat the test. In many cases, the result will be positive on the second or third test. In some patients, an empiric trial of the KPU protocol may be indicated despite repeated negative KPU tests, and this often leads the patient to higher ground.
WBC (not RBC) intracellular zinc may be a useful tool for exploring the potential for zinc deficiency where it matters most - in the white blood cells.
Other laboratory indicators that may be suggestive of KPU include the following:
- WBC < 5000/mcL (due to low levels of zinc)
- High LDL / Low HDL
- Low normal alkaline phosphatase (<60U/L)
- Low omega-6 fatty acids in red cell membrane test
- Low taurine in amino acid profile
- High MCV
- Low glutathione
- Low ATP
- WBC and RBC zinc and manganese levels may be normal while biopsies from bone and CNS are completely deficient.
- Bone biopsies are a reliable predictor of KPU. Severe deficiencies of zinc, manganese, lithium, calcium, magnesium, and molybdenum are often found.
Alkaline phosphatase (ALP) is a zinc and magnesium dependent enzyme. When someone is consuming adequate magnesium and is still presenting with low ALP, zinc deficiency is a likely consideration, and this may represent another indication for KPU. When ALP is below 55, zinc deficiency can be suspected; when below 40, it is likely.
A consequence of KPU is low glutathione and low ATP. In the realm of chronic illnesses, low reduced glutathione and low ATP are common and should alone trigger the suspicion that KPU may be a factor.
Page 1, 2, 3
|
![]()
![]()
![]()
![]()







