Page 1, 2, 3, 4
It takes a rare and exceptional lab staff to visualize Babesia on a slide. As the author of six Babesia books and other tick infection writings, I have sent many Babesia and tick infection cases for blood smear testing. I have had antibody-positive and PCR (DNA)-positive Babesia patients, yet the most respected routine labs never see the Babesia organisms on a smear. Nackos had a good laboratory team. (Perhaps the blood Babesia volume was showing infection in a high percent of cells, as seen in Figure 4).
Figure 4: This European woman had been treated with routine Babesia medication by infection specialists. Do you think that the treatments and duration worked? This is a deadly number of parasite-filled red blood cells.
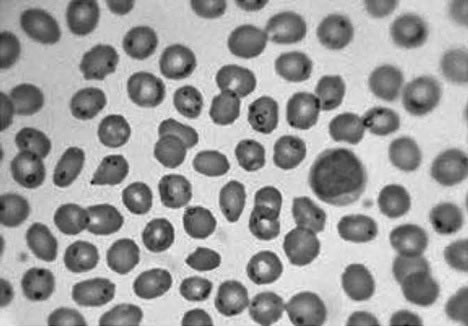
Babesia microti can cause deadly hemolytic anemia and/or dangerously low platelet levels (thrombocytopenia) per Nackos. I would add that it can also alter other labs such as decreasing white blood cell levels to 1200 to 5000. Altered red blood cell (RBC) numbers can also hint at the presence of Babesia.
A Cancer Caused by Babesia
We published a functional cure for hypereosinophilic syndrome (HES), a blood cancer, from patient care provided in 1999–2000.15 Over 250 physicians missed the primer of this blood eosinophil cancer – a Babesia infection.16
Diagnosis
Direct testing for Babesia at the major world labs fails both patients and the doctors who treat them. Both antibody testing and DNA (PCR) testing at the largest world laboratories have little sensitivity. No laboratory tests are perfectly sensitive; however, the best and most advanced laboratory for Babesiaantibody testing, PCR, and smear visualization is IGeneX. I am often perplexed when someone tests for "Lyme" at IGeneX and no other infection, such as babesiosis, is explored. I have had patients who were positive for Babesia and Bartonella with no Lyme disease.
Further, another trouble in diagnosis is from the impact of Bartonella on Babesia antibody testing. Bartonella is more common than either Lyme or Babesia, and it is immunosuppressive, so at times in diverse ways it alters direct and indirect testing results for Babesia.17-22
One simple tool used to diagnose Babesia is to start treatment with Babesia medications. The more treatment given the patient, the more likely you are to get a positive direct – or indirect – Babesia test. Physicians are trained not to treat without good evidence of a positive diagnosis. Unfortunately, that means using routine local labs that will almost always miss the Babesia. However, once the physician cancer patient in our HES study was exposed to two strong Babesia medication options and the semisynthetic herb artesunate – not the weaker artemisinin – his Babesia antibody test converted from negative to positive, and some other indirect chemical markers of the presence of Babesia changed as Babesia organisms were killed.
Zhao provides a useful example of the defect of PCRs in a Babesia transfusion death.23 A patient given Babesia-infected blood died from the Babesia. Although tragic, we should not be surprised since only last year Goodell reported that no Babesia test exists or is utilized to screen blood donations in the US.24
In investigating this man's death, 13 blood donors were tested for B. microti. All donors were negative by PCR. However, one donor living in New Jersey had a profoundly elevated B. microti antibody titer (1:1024).
FISH Testing
IGeneX has a test that helps visualize Babesia duncani and microti. It uses a probe that has one end that attaches to the organism and another end that is vividly visualized to help a microscope expert see the Babesia. However, as you recall, seeing Babesia is an activity that takes more than an hour unless you are infected with a dangerously high level of Babesia organisms. Our position is that this is a good test to determine quantity. If you are positive, you likely have a high level of Babesia. This does enhance examination of a blood smear, but roughly 85% of the positives will be missed. Babesia is missed by LLMDs and infection physicians because of their reliance on laboratory results rather than the art of diagnosis which uses a good patient history and examination.25 This overreliance on lab results is one of many reasons for the failure of LLMDs and infection physicians in tick infection care. Lyme is seen as the "core infection," and Babesia is a coinfection. This is an error. Typically, people who have a positive FISH become negative with effective care. This does not mean that they are cured; it means that they are losing body load, making Babesia harder to see, even with this smart enhancement tool (FISH). I do believe that the test is worth ordering if the patient can afford it. (Figure 5 is a black-and-white picture of the FISH test showing various types of Babesia inside red blood cells.)
Figure 5: The FISH image, in black and white, enhances the visibility of Babesia microti and duncani. About 15 different Babesia forms are shown. This was supplied by Dr. J. Shah of IGeneX.
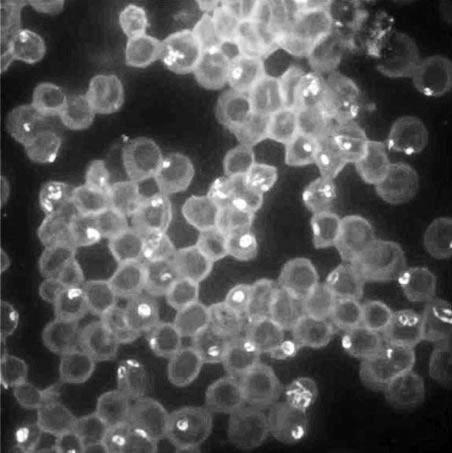
FL1953 or Protomyxzoa Rheumatica: The Babesia-Like New Protozoan
This protozoan was sent to the CDC, which reported that it was a protozoan and not malaria or Babesia. The agency could not identify it. Dr. Stephen Fry reports that many studies are being conducted with the goal of publication in a close time frame. We believe that the DNA sequencing done by the Fry Laboratory genetics experts shows a new form of protozoan that is a biofilm engine. For more information, see my summary article at http://www.personalconsult.com/posts/FL1953.html. We also offer options for treating FL1953 biofilm issues in the best-selling biofilm textbook in the world.26 (Figure 6 shows hundreds of black tiny red blood cells with a large white collection of complex biofilm jelly generated by FL1953.)
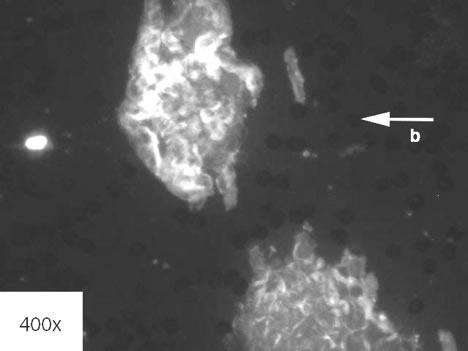
Figure 6: FL1953 or Protomyxzoa rheumatica is shown creating biofilm. The CDC reports that it is a genetically unique protozoan per Dr. Stephen Fry of Fry Laboratory. The small black circles marked by a "b" arrow are hundreds of red blood cells. Notice the two massive white biofilm balls that are approximately 100 times the size of a red blood cell.
Source of image: Fry Laboratory.
Variation in Diagnosis and Treatments
100 years ago, before antibiotics, Rocky Mountain spotted fever (RMSF) was death to between 20% and 80% of the people who contracted it – the difference in death rate depended on a small difference in location. The next town could have a radically different outcome. My appeal is that we know that Babesia species have many strains. The variation of strains from state to state determines some of the variation in symptoms of patients from different areas of the country.
Treatment
One of the disasters in treatment is based on the variation we mentioned with RMSF. Baseline pre-2015 treatments were weak and showed ignorance of the power of Babesia – it is vastly harder to kill than malaria. Therefore, simply plugging in malaria herbs or drugs can fail. Modern treatments might be founded on a famous paper that seemed to define perfect Babesia care rigidly for 15 years in infection care both by infection physicians and LLMDs.27
In 2000, Krause, who had published concerns of suboptimal results with clindamycin and quinine therapy, reported low side effect and high success with a short course of atovaquone (Mepron) liquid at a dose of 1500 mg/day used in the presence of azithromycin (Zithromax) 500 mg/day.28,29 While the addition of another tool in the treatment of Babesia should be welcomed, many aspects of this approach are found to be flawed in 2015.
1. A review of Babesia species that infect humans shows immense variation, and the idea of one dosage for everyone is limited medical science. The infinite complexity and uniqueness of your body as it changes each month in hundreds of systems confuses Babesia treatment with the purity of basic arithmetic.
2. Human immune systems are complex and never clones in which everyone in a city could be given the same exact treatment for the same duration.
3. The determination of the presence of infections such as Babesia in ticks and human bodies is markedly limited. (Figure 4 [p. 68] is a picture of a patient after this treatment who suffered severely due to its ineffectiveness.)
4. Some patients are extremely sensitive to the atovaquone and they do not have an allergy. They experience a dose flaw. It is too effective. Not everyone can handle 1500 mg per day.
5. The issue of resistance to atovaquone is a concern in 2015.30,31
6. Ignoring the resistance question, another option is that some people need a higher dose, as correctly advocated to me by a kind physician, Richard Horowitz, over 10 years ago.32,33
7. The role of azithromycin and the dose used seems arbitrary. We can easily measure blood levels and on 500 mg/day the range of levels are highly variable.
Page 1, 2, 3, 4
|
![]()
![]()
![]()







