


July 2004
by Gina L. Nick, PhD, ND
"Functional foods," "nutraceuticals," "designer foods" and "medicinal foods" are terms that describe foods, and key ingredients isolated from foods, that have non-nutritive or tertiary functional properties. Researchers, healthcare practitioners, laypersons, and the popular media use these words interchangeably. The purpose of this article is to detail valid scientific and pertinent clinical information on the effects of toxic exposure on breast cancer risk and whole foods recognized for their ability to detoxify chemicals from the body.
Breast Cancer, Toxic Exposure and Detoxification
Breast
cancer is second only to lung cancer as the most common cause of cancer
mortality in the US. Further, in the year 2000 alone, 182,000
new cases of breast cancer were diagnosed and there were 40,800 associated
female deaths in the US as a result. In fact, breast cancer is the leading
cause of death in women between the ages of 35 and 54.1 A key contributing
factor, that is supported by clinical research, to the onset of breast
is toxic exposure, in the form of synthetic hormone replacement therapy
and chemicals in the food, air and water supply.
The Toxic Effects of Synthetic Hormone Replacement Therapy
A woman's chance of developing breast cancer significantly increases
with age (Table 1).1
Table 1. Breast cancer risk as it relates to a woman's age.
| Age | Breast Cancer Risk |
| By 30 | 1 out of 2,212 |
| By 40 | 1 out of 235 |
| By 50 | 1 out of 54 |
| By 60 | 1 out of 23 |
| By 70 | 1 out of 14 |
| By 80 | 1 out of 10 |
| By 90 | 1 out of 8 |
As a woman ages, she will naturally
approach menopause and the cessation of ovarian function, increasing
her chances of taking hormone replacement
therapy (HRT) to reduce symptoms commonly associated with menopause and
to prevent the onset of heart disease and osteoporosis. In fact, surveys
by the North American Menopause Society show that about a third of US
women ages 45 to 65 — some 16 million women — use hormone supplements,
either estrogen alone or combined with progestin. Disturbingly, HRT increases
a woman's risk of breast cancer, sometimes by more than 50% and,
we now know, it fails to prevent heart disease and in fact increases
a woman's chance of developing a life-threatening blood clot or
a stroke. The now famous study2 published in 2002 in the Journal
of the American Medical Association provided definitive evidence that the use
of combined HRT (meaning conjugated equine estrogens and medroxyprogesterone
acetate (PremPro) significantly increases a woman's chance of
developing breast cancer. This was a randomized, placebo-controlled trial,
which was a component of the Women's Health Initiative, a multi-part
study begun by the National Institutes of Health that enrolled more than
160,000 postmenopausal women at 40 US medical centers between 1993 and
1998.
The purpose of the study was to investigate the efficacy and safety of
long-term hormone replacement therapy in preventing diseases in postmenopausal
women
such as heart disease, breast and colorectal cancers, and osteoporosis. Over
16,000 menopausal women with an intact uterus participated in this trial, receiving
conjugated estrogens (at .625 mg/day) plus medroxyprogesterone acetate (at
2.5 mg per day) combined in one tablet or placebo. Considered one of the largest
studies of women's health ever taken, it made headlines when the review
committee for the study halted the study three years early (final results were
due out in 2005). They determined that the number of cases of invasive breast
cancer in the combined HRT group crossed the boundary established for the study
as a signal of increased risk.
For example, the estrogen/progestin therapy used in this trial resulted in
a 26% increase in breast cancer. The combined HRT also resulted in:
- 41% increase in strokes
- 29% increase in heart attacks
- Doubled rates of blood clots in legs and lungs
- 37% fewer incidents of colorectal cancer
- 33% fewer hip fractures
- 24% fewer total fractures
It is interesting to note that other parts of the WHI trial, including a study evaluating the effects of estrogen alone (Premarin), in postmenopausal women without a uterus, continued. This study continued irrespective of the fact that a cohort observational study involving over 44, 000 postmenopausal women without a uterus, published in same issue of JAMA (334-341) by Lacey et al.3 found that estrogen-only HRT resulted in a 300% increase in ovarian cancer. Finally, in March of this year, the NIH discontinued this phase of the trial because estrogen had no effect on preventing heart disease after 7 years of continuous use, and it was shown to increase the risk of stroke. A separate report points to "probable" dementia and/or mild cognitive impairment associated with estrogen-alone therapy.4
Toxic Exposure from the Air, Water, and Food Supply
Beyond the toxic effects of synthetic HRT, which women have been exposed to
for decades, environmental chemicals in the air, water and food supply have
a well-documented effect on breast cancer risk. For the last 40 years, substantial
evidence has surfaced on the hormone-like effects of environmental chemicals
such as pesticides and industrial chemicals in humans.
Since the creation of organic and inorganic chemicals in the late 19th century,
the global community has faced an exponential rise in the production and subsequent
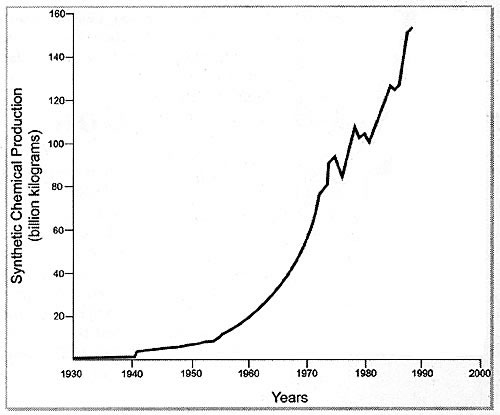
exposure to such environmental chemicals.5 Between the 1940's and the
1990's synthetic chemical production has risen from 1 billion kilograms
to 160 billion kilograms. (Figure 1).6
Figure 1. Graphic representation of the exponential rise in production of environmental chemicals since the 1940s.6
Many of these chemicals are often referred to as xenoestrogens. Xenoestrogens
are environmental compounds with estrogen-like activity that may cause
hormone-related cancer in some individuals. The endocrine and reproductive
effects of these chemicals include their ability to:
1. Mimic the effect of endogenous hormones
2. Antagonize the effect of endogenous hormones
3. Disrupt the synthesis and metabolism of endogenous hormones, and
4. Disrupt the synthesis and metabolism of hormone receptors.7
Unfortunately, but not surprisingly, the discovery of hormone-like activity
of these chemicals occurred long after they were released into the environment.7
As it relates to breast cancer, this is especially true of the principal metabolite
of DDT (DDE), which remains in the body fat for years following exposure. In
a study of 14,000 women, published in the Journal
of the National Cancer Institute,8
breast cancer was strongly associated with exposure to organochlorine insecticides,and
especially DDE. Confirming these results, researchers9 found that DDE and Red
Dye No. 3, a food colorant, markedly increase proliferation in human breast
cancer cells that are estrogen receptor-positive. We now know that exposure
to pesticides, dyes, and pollutants that mimic the growth promoting effects
of estrogen can indeed initiate the onset of breast cancer. So, let us take
a look at just how prevalent exposure to xenoestrogenic chemicals in our food
is.
The Prevalence of Xenoestrogens in the Food Supply and Foods to Help
Augment Their Effects
There is an ongoing Food and Drug Administration (FDA) program known as the
Total Diet Study (TDS), sometimes called the Market Basket Study. This program
was originally prompted in 1961 by public concern over radioactive contamination
of foods following atmospheric testing of nuclear weapons.
The purpose of the program/study is to determine levels of various pesticide
residues, contaminants, and nutrients in foods, in order to estimate the amount
of these chemicals that are being ingested by specific age sex groups in the
United States population. To do this, the FDA has personnel purchase foods
from grocery stores four times per year, one from each of four geographic regions
of the country. Each "Market Basket" is a composite of like foods
purchased in three cities in a given region. They then go on to prepare the
foods as they would normally be prepared in the average household, and they
analyze it.
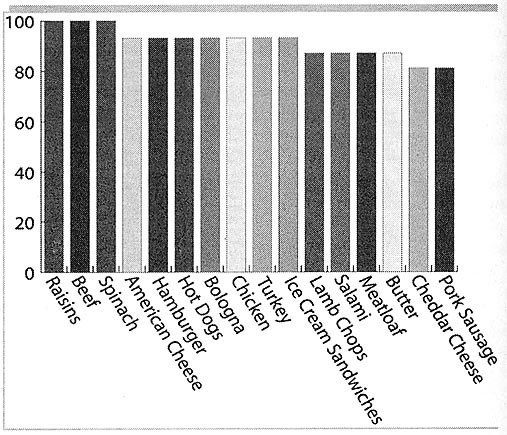
Amazingly, DDE was found in 100% of the samples of raisins, spinach (fresh
and frozen), chili con carne (beef and bean), and beef that they analyzed.
It was found in 93% of the samples of American processed cheese, hamburger,
hot-dogs, bologna, collards, chicken, turkey and ice cream sandwiches. It was
found in 87% of the samples of lamb chops, salami, canned spinach, meatloaf
and butter. It was found in 81% of the samples of cheddar cheese, pork sausage,
quarter-pounders, white sauce, and creamed spinach (Figure 2).
Figure 2. Results of the FDA Total Diet Survey — %
of samples that contain DDE
Since 1976, the Environmental Protection Agency (EPA) has been running the National Human Adipose Tissue Survey that provides further evidence of the presence of xenoestrogens in the environment and their direct effect on our bodies. This is an annual program whereby the EPA collects and chemically analyzes a nationwide sample of adipose tissue specimens for the presence of xenoestrogens. The tissue is analyzed for organochlorine pesticides, PCBs, dioxins and furans, volatile organics, semivolatile organics, and trace elements. Not surprisingly, DDE was found in 91-98% of the samples tested. OCDD was found in 100% of the adipose tissues sampled—and OCDD is a dioxin.
Dioxins and Breast Cancer
The main dietary source of dioxin is meat and dairy products. We know that
dioxin latches onto the aryl hydrocarbon receptor, through which it gains
access to cells and has as great an effect on breast cancer cell growth as
17 betaestradiol, a recognized and known cause of breast cancer cell growth.
Providentially, there are foods that help to brighten this grim reality of
living in a world where xenoestrogens are ubiquitous and breast cancer continues
to take the lives of far too many women each year. Broccoli, and in particular,
the indole 3 carbinol (I3C) found in broccoli, interferes with xenoestrogens,
including DDT and dioxin by blocking access to cells via the aryl hydrocarbon
receptor. Consequently, I3C cuts the rate of DNA damage in breast tissue exposed
to chemicals by nearly 92%.10
There are other components, such as d-glucarate in broccoli, that support the
detoxification of xenoestrogens and that are of equal if not more importance
to breast cancer prevention as I3C. However, if you do choose to recommend
or carry I3C as a dietary supplement in your practice, rather than recommending
an increase in the consumption of broccoli, I suggest using a product that
is housed in a glass versus plastic bottle. There is research that now suggests
a direct effect of Bisphenol A (BPA) on estrogen receptors. BPA is widely used
in the production of transparent PET bottles and in the lining of tin cans
and it represents another xenoestrogen showing estrogen-like activity,11 with
researchers cautioning that it may contribute to breast cancer risk.
Heterocyclic Amines and Breast Cancer
Heterocyclic amines (HA) are another class of xenoestrogens associated with
breast cancer risk. Results from the famous Iowa Women's Health Study12
found that women who consistently eat well-done steak, hamburgers and bacon
have a 4.62 fold increased risk of breast cancer. Cooking foods at high temperatures
causes the formation of HA's which are linked to breast cancer. And
interestingly enough, even grilled salmon contains sufficient levels of HA's
to cause gene mutation.
Women who have a polymorphism, or genetic variation, of N-acetyltransferases
(NAT) alleles are at a higher risk of damage from HA's.13,14 NAT are
major enzymes of breast tissue that activate aromatic and heterocyclic amines,
such as those found in cigarette smoke and well-cooked red meat. Researchers
found that certain polymorphisms, or genetic variations, of NAT alleles found
in humans are significantly more highly correlated with breast cancer risk
due to smoking and red meat consumption than others. These alleles code for
the "rapid/intermediate acetylator phenotype" in which heterocyclic
amines are more quickly activated, increasing the risk of toxic DNA damage
leading to cancer. Women with the rapid/intermediate acetylator phenotype may
be at significantly higher risk for breast cancer if they smoke and consume
meat cooked at high temperatures.
There is an endless supply of xenoestrogens in the environment. Even at small
doses, where there is no documented effect on human health, these chemicals
do in fact cause great damage to the body, when they are combined.
Combined No-Observed-Effect-Concentrations of Environmental Chemicals
(NOECs)
A study completed by Dr. Silva and colleagues15 demonstrated that estrogenic
chemicals below their NOECs act together to produce significant effects. These
researchers tested multi-component mixtures of eight weak environmental chemicals
known to bind to estrogen receptors, including hydroxylated polychlorinated
biphenyls, benzophenones, parabenes, bisphenol A and genestein. The mixtures
were prepared so that no one chemical would contribute disproportionately to
the overall effect based on their known individual potencies. Concentrations
of the individual components ranged from 0.004 µM to 1.04 µM. The
researchers measured the estrogenic effects of the low dose chemical mixture
utilizing the Yeast Estrogen Screen. Using this reporter gene assay, they first
demonstrated that each chemical tested activated the genetically modified yeast
cells' estrogen receptor protein.
The additive combined effects of the weak estrogenic compounds were then calculated
using four separate models-concentration addition, toxicity equivalency factors,
effect summation, and independent action. From these estimations, the researchers
determined that the concentration addition and toxicity equivalency factor
approach were valid methods for the calculation of additive mixture effects,
as there was excellent agreement between prediction and observation. Remarkably,
there were substantial mixture effects even though each chemical was present
at levels well below its NOEC. The researchers concluded that estrogenic agents
are able to act together to produce significant effects when combined at concentrations
below their NOECs. The results of this study highlight the limitations of assessing
chemical toxicity on a chemical-by chemical basis. Conventional risk assessments
of toxic environmental chemicals ignore the likelihood of combined actions,
which will almost certainly lead to significant underestimations of risk.
In reality, humans and wildlife are exposed to compound, typically nonspecific,
mixtures of chemicals. Fortunately, there are whole foods that, when consumed
as a regular part of the diet, reduce the adverse combined effects of NOECs
of environmental toxic chemicals, as described in the Silva study.
Whole Foods that Support Detoxification
A review of the epidemiological studies to date that demonstrate an inverse
correlation between high vegetable consumption and cancer risk revealed that
57% of all such studies show a protection against breast cancer with high
vegetable intake. The relative median risk (low vs. high consumption of vegetables)
was 1.3.16
Likewise, a high intake of fruits and vegetables correlates with decreased
breast cancer risk in premenopausal women. However, supplements of vitamins
A, C, and E, and multivitamins, were not associated with overall risk, supporting
a whole food philosophy.17 Fruits and vegetables contain numerous tertiary,
non-nutritive compounds including isoflavones, dithiolthiones, indoles, flavonoids,
and phenols, all of which have proposed mechanisms of action and relative sites
along the normal to abnormal cell transformation pathways that inhibit carcinogenesis
and provide chemoprotection, sometimes by supporting the actions of the Human
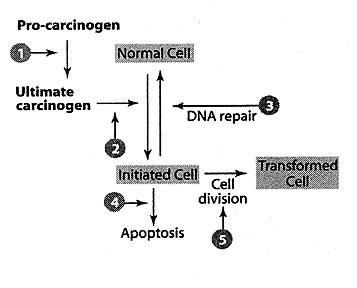
Detoxification System (Figure 3).
Figure 3 — The potential mechanisms and sites for the inhibition of carcinogenesis by protective tertiary compounds found within a whole food matrix.
With regard to the detoxifying effects of whole foods, Staack et al.18
examined the effects of a mixture of glucosinolate breakdown products
from Brussels sprouts (a member of the Cruciferous family of vegetables),
on the induction of liver detoxification enzymes in rats. The mixture
(full strength, 60%, and 20%) elevated levels of cytochrome P450 1A (CYP1A),
glutathione-S-transferase (GST), quinone reductase (QR), glutathione
reductase (GR), and glutathione (GSH) in a dose dependent manner, supporting
the hypothesis that glucosinolates found in green vegetables are important
in the regulation of hepatic detoxification.
The following Brussels sprout glucosinolate breakdown products and amounts
were used in the mixture fed to the rats:
- Indole-3-carbinol (I3C; 56 mg/kg)
- Iberin (38 mg/kg)
- Phenylethylisothiocyanate (PEITC; 0.1 mg/kg)
- Cyanohydroxybutene (crambene; 50 mg/kg)
The amounts reflect the proportionate amounts of each glucosinolate compound
found in Brussels sprouts standardized to 50 mg crambene/kg (induces glutathione
without toxic effects). It is important to note that in this study the individual
glucosinolate breakdown products were also tested. While indole-3-carbinol
(I3C) was the only glucosinolate in the mixture to significantly increase
enzyme activity, the glucosinolate mixture containing I3C was considerably
more effective,
supporting a synergistic mechanism of action between the compounds. This
suggests that bioactive molecules ingested as part of a complete nutritional
regimen
may be considerably more effective than the isolated active principles used
alone.
Isothiocyanates have also been shown to act as anticarcinogens by inducing
detoxification of environmental mutagens.19 Sulforaphane blocked 7,12-dimethylbenz(a)-anthracene-induced
mammary tumors in rats20 and broccoli extract was a potent inducer of detoxification
enzymes in a mouse hepatoma cell assay, probably due to sulforaphane as well.21
Fifty percent of people completely lack the glutathione-S-transferase M1
(GSTM1) enzyme due to a homozygous gene deletion. This enzyme is responsible
for the
rapid conjugation of isothiocyanates to glutathione for excretion (Phase
II). Lin et al.19 hypothesized that people with this mutation would maintain
higher
levels of isothiocyanates in the body due to decreased excretion and should
show a lower incidence of colorectal adenomas, the precursors of colorectal
cancer, if isothiocyanates are indeed anticarcinogenic. The researchers found
that broccoli and kale, but not cabbage, cauliflower, or Brussels sprouts,
were significantly associated with lower prevalence of colorectal carcinomas
in a sample of nearly a thousand people (459 adenoma cases and 507 controls
sampled from patients undergoing cancer sigmoidoscopy screening in southern
California). The presence of the GSTM1 null genotype alone did not significantly
correlate with the occurrence of colorectal carcinoma. However, the GSTM1
null genotype did correlate with a significant reduction of incidence of
colorectal
carcinoma when it was covaried with broccoli and total cruciferous vegetable
consumption (p=0.001 and p=0.02, respectively). The lowest incidence of colorectal
carcinoma occurred in GSTM1 null individuals in the highest quartile of broccoli
consumption, supporting the hypothesis that isothiocyanates in crucifers
may be excreted more slowly in urine in GSTM1 individuals. However, neither
urinary
nor serum isothiocyanate measurements were taken in the subjects, so other
mechanisms cannot be ruled out. It is clear from the body of research available
that consumption of higher levels of cruciferous vegetables is indicated
for reducing the risk of breast cancer.
Another cruciferous vegetable that has specific effects on breast cancer
risk is broccoli. In addition to its glucosinolate content, broccoli contains
a
particularly high level of D-glucarate (broccoli contains the highest percentage
of any plant studied), a compound that confers a protective effect against
breast cancer. D-glucorate also supports detoxification and the removal of
xenoestrogens. It is currently being used in a phase I human trial at Memorial
Sloan-Kettering Cancer Center in women at high risk for developing breast
cancer. This study is in collaboration with the National Cancer Institute
and the National
Institutes of Health. Yet another member of this same family of vegetables
is cabbage. Supporting the whole food philosophy, we know that in addition
to glucosinolates, cabbage contains other compounds that have a recognized
effect on breast cancer. Some known medicinal constituents in cabbage include:
- 4-Me-glucobrassicin
- Folate
- 4-OH-glucobrassicin
- Glutamine
- Sinigrin
- Flavonoids
- Glucoiberin
- Isothiocyanates
- Phenolic compounds
- Indole-3-carbinol
Folic acid, present in cabbage, works with vitamin B12 to enhance DNA
Methylation in the conversion of estrogen to the more protective 2
hydroxyestrone metabolite.
Cabbage also is a rich source of glutamine. When glutamine levels drop,
intestinal epithelial cells and lymphocytes begin to lose function, compromising
the
integrity of the epithelium and leaving the intestine vulnerable to microbial
translocation
(passage of bacteria or toxins into the bloodstream via the intestinal
wall). Gut-associated lymphoid tissue (GALT) also requires glutamine for optimal
function. GALT comprises the Peyer's patches and lymphoid follicles scattered
throughout the intestinal mucosa. Maintenance of immune function and a
healthy
intestinal tract is vital to supporting one's ability to eliminate environmental
toxins from the body.
Vegetables that are rich in chlorophylls are also beneficial in supporting
the detoxification of environmental chemicals that contribute to breast
cancer development. Chlorophylls form molecular complexes with toxins,
inactivating
them by preventing their binding to DNA and cellular receptors.22 Chlorophylls
also specifically inhibit cytochrome P450 detoxification activity.22 It
is important to keep in mind that chlorophyll-rich vegetables, such as
broccoli,
Brussels sprouts and kale, are also rich in indole-3- carbinol, calcium-d-glucarate,
and other compounds recognized for their actions in preventing breast cancer
and supporting the elimination of cancer-causing environmental toxins.
Finally, flaxseed, the richest known source of plant lignans (a sub classification
of phytoestrogens), has been shown to have chemoprotective effects in women.
Some of its effects may be mediated through its influence on endogenous
hormone production and metabolism. Two competing pathways in estrogen metabolism
involve production of the 2-hydroxylated and 16 alpha-hydroxylated metabolites.
Because
of the proposed differences in biological activities of these metabolites,
the balance of the two pathways has been used as a biomarker for breast
cancer
risk. Researchers23 examined the effects of flaxseed consumption on urinary
estrogen metabolite excretion in postmenopausal women. What they found
was that postmenopausal women eating 5 to 10 g of ground flax per day showed
an increase in urinary 2-hydroxyestrone excretion, in a linear dose-response
fashion
suggesting a chemoprotective role for flax seeds (p<0.0005). What is also
promising about flax seeds is that they help to improve the cardiovascular
risk profile in postmenopausal women. Given the toxic effects of synthetic
hormone replacement therapy, which is often recommended to augment cardiovascular
risk in these women, it is hopeful to know that there are foods which not only
offer breast cancer protection, but also help to prevent the need to take in
something as toxic to a woman's body as synthetic hormone replacement
therapy.
Researchers24 studied the association between dietary phytoestrogen intake
and metabolic cardiovascular risk factors in postmenopausal women. For
this purpose, 939 postmenopausal women were included in the cross-sectional
study.
Postmenopausal women who consumed a significant amount of lignan-rich foods
had less weight concentrated around their waist (lower WHR) than those
who ate little or none suggesting an improvement in metabolic cardiovascular
risk profile.
Final Thought
Breast cancer has strong environmental factors (such as toxins in the food,
air and water supply, and synthetic HRT) and strong genetic factors. We ought
to view breast cancer, and its causes, as a matter of nature and nurture,
rather than nature versus nurture. We should not view cancer as having a
single "cause," but understand that a combination of these
factors brings about cancer. There must be a critical number of "hits" to
a person's DNA that occur before we see the onset of cancer. By "hits" I
mean damage. Whether it be hits that we are born with (genetic predisposition),
or hits that occur after we are born (such as environmental toxins damaging
our DNA). Knowing this, I will add that it is my belief that preventing or
augmenting the effects of "hits" that we receive after we are
born is most effectively accomplished through the use of foods, such as broccoli,
Brussels sprouts and other chlorophyll-rich foods, such as cabbage and flax
seeds.
The Commonwealth Scientific and Industrial Research Organisation (CSIRO)
held a conference in Melbourne entitled "Beyond the Human Genome." in
February of 2002. And what was reported was that research in the CSIRO and
elsewhere has shown that we can reduce our levels of genetic damage by consuming
optimum levels of vitamins and minerals from our foods. In fact, according
to Dr. Bruce Ames25 of the University of California at Berkley, who researches
the effects of micronutrient deficiencies on gene health; Deficiency of vitamin
B12, folic acid, B6, niacin, vitamin C, vitamin E, iron or zinc, appears to
mimic radiation in damaging DNA caused by single- and double-strand breaks,
oxidative lesions or both…half of the population may be deficient in
at least one of these micronutrients.
Studies done by Dr. Ames and many others, some of which presented their material
at the Melbourne conference, have shown that gene damage through inappropriate
diet may be as significant as genetic mutation brought about by toxic chemicals
and radiation. Imagine the prevalence of damage ("hits") caused
by inappropriate diet and a toxic environment.
![]()
References
1. Nogueira, S. and S.E. Appling. Nurs Clin
North Am. 2000;35(3):663-669.
2. Women's Health Initiative Trial JAMA 2002; 288:321-333.
3. Lacey, J. et al. JAMA 2002;288:334-41.
4. http://www.nhlbi.nih.gov/new/press/04-04-13.htm
5. Flegal K., et al. Int J Obes Relat Metab
Disord 1998;22(1):39-47.
6. Baillie-Hamilton, P. J Alt Comp Med 2002;8(2): 185-192.
7. Sonnenschein C., Soto A. J Steroid Biochem
Mol Biol 1998; Apr;65(1-6):143-50.
8. Dewailly E. , et al. J Natl Cancer Inst 1994; Feb 2;86(3):232-4
9. Dees C., et al. 1997; Environ Health Perspect Apr;105 Suppl 3:625-32.
10. Frieson, H. et al. Food Chem Toxicol 2000;38(1):15-23.
11. Recchia, A. et al. Food Addit Contam.
2004 Feb;21(2):134-44.
12. Zheng, W. et al. J Natl Cancer Inst 1998;90(2):1724-9 & 90(22):1687-9.
13. Deitz, A. C. et al. Cancer Epidemiol Biomarkers
Prev 2000; 9(9):
905-910.
14. Zheng, W. et al. Cancer Epidemiol Biomarkers
Prev 1999; 8(3): 233-239.
15. Silva, E. et al. Environ Sci Technol 2002;
Apr 15;36(8):1751-6.
16. Block, G. et al. Nutr Cancer 1992; 18(1): 1-29.
17. McKeown, N. Nutr Rev 1999; 57(10): 321-324.
18. Staack, R. et al. Toxicol Appl Pharmacol. 1998; 149(1): 17-23.
19. Lin, H. J. et al. Cancer Epidemiol Biomarkers
Prev 1998;7(8): 647-652.
20. Zhang, Y. et al. Proc Natl Acad Sci USA 1994;91(8): 3147-3150.
21. Zhang, Y. et al. Proc Natl Acad Sci USA 1992;89(6): 2399-2403.
22. Yun, C-H. et al. Carcinogenesis 1995;16(6): 1437-1440.
23. Haggans, C.H. et al. Nutr Cancer 1999;33(2):188-95.
24. de Kleijn, et al. J Nutr 2002 132(2):276-82.
25. Ames, B. Mutation Research 2001;475: 7-20.
![]()
Gina L. Nick, PhD, ND
Chief Scientific Officer at Longevity Through Prevention, Inc.
Phone: 866-587-4622 x70
Fax: 866-587-4622
E-mail: drgina@LTPonline.com
P.O. Box 6936
Laguna Niguel, California 92607
www.LTPonline.com
Search
our pre-2001 archives
for further information. Older issues of the printed magazine are also
indexed for your convenience.
1983-2001
indices ;
1999-Jan. 2003 indices
Once you find the magazines you'd like to order, please use our
convenient form, e-mail subscriptions@townsendletter.com,
or call 360.385.6021 (PST).
All rights reserved.
Web site by Sandy Hershelman Designs

