Page 1, 2, 3, 4
Salivary Hormone Tests for Adrenal Stress Disorder
The primary marker for hypothalamus-pituitary-adrenal (HPA) activity in humans is cortisol, having complex and diverse effects throughout the body.50,51 Salivary cortisol measurements have been in use since the 1960s. The majority of studies published using salivary cortisol involved its application in studying the stress response and psychoneuroendocrinology, rather than for the clinical evaluation of patients.52,53 The steroid hormones most readily measured in saliva are: estrogens (estradiol, estrone, and estriol), progesterone, androgens (DHEA, testosterone), and cortisol.54
It is accepted that blood cortisol levels rise in response to physical, chemical, psychological and thermal stressors, and that there is a reliable direct correlation between blood cortisol and salivary cortisol levels.55,56 It is worth noting that the World Health Organization uses saliva testing to study human hormone levels around the world.5,32
The biologically active component of the HPA axis is plasma free cortisol that is in equilibrium with salivary cortisol.57 There are a variety of approaches to obtain saliva for the measurement of cortisol, including expectoration, passive drool, aspiration (particularly in infants), and chewing on a cotton or polyester swab using commercial devices.
Low cortisol levels are not mere artifacts of measurement or sampling methods, a variety of different technologies have shown low cortisol levels in saliva, urine, and blood in many populations with stress-related disorders.57 Physical pain and other functional neuromuscular disorders are distressing, and these too have been associated with low cortisol.58,59
Because cortisol release peaks in the morning during the HPA axis circadian rhythm, it is theoretically possible that assessment of a subnormal morning cortisol might be diagnostic for adrenal insufficiency. Abnormal diurnal rhythms were assessed and reported for each of the participants in our study. The problem with assessing only morning cortisol is the wide range of morning serum and salivary cortisol in normal participants.6,60,61
In addition, samples of saliva in our cohort were analyzed for DHEA levels. Dehydroepiandrosterone, the most abundant steroid hormone in the body, has been shown to significantly buffer the stress response.62–64 It was expected that following the AK physical assessment and patient history indicating ASD, that waking salivary cortisol and DHEA levels would be abnormal. The DHEA level is an indicator of the functioning of the area within the adrenal glands that produces the sex hormones (the zona reticularis).
Cortisol's stability in saliva at room temperature for at least a week allowed samples, after collection, to be mailed to the laboratory by standard postal service.65–67
We found that testing hormones in saliva was convenient, painless and therefore less stressful and less expensive than blood tests. More importantly, saliva contains the free, "bioavailable" fraction of steroid hormones that have moved out of the bloodstream and into the tissues. Furthermore, the stress caused by a conventional blood draw can alter test results. For salivary hormone determinations, the home collection kit allows for optimal collection times.
Can Internal Medicine and Physical Medicine Interact In This Way?
Exposure to taste elicits a variety of immediate neurological, digestive, endocrine, circulatory, and renal responses throughout the body and has been called the cephalic or pre-absorptive response.68,69 Of key importance are the skeletal muscles, which are affected through the action of foods upon the taste receptors.70 The large mass of skeletal muscle in the body (60% of the body's weight) plays an integral role in blood sugar and insulin metabolism, with the latter disposing of approximately 50% of the increased postprandial blood glucose into muscle cells for use as energy, and up to 10% for conversion to glycogen.13
The sensory receptors embedded in lingual epithelium are used to distinguish chemical compounds that are potentially nutritive (e.g., salts, sugars, proteins, carbohydrates, fats, and so forth) from those that are potentially harmful (e.g., bitter-tasting plant alkaloids, allergens, toxins, etc.).17,68 Such judgments help the gastrointestinal (GI) system to process substances in the mouth by causing the organism to salivate, masticate, swallow, or expel, as well as to release insulin and other peptides for digestion. Man and animals rapidly associate post-ingestion effects with the flavor of food or nutrition. If there are adverse physiologic effects from eating an item, a learned response of aversion to repeating the act is rapidly associated with the flavor and odor of the foodstuff so that the act will not be repeated.17
The taste buds also have an effect upon blood sugar levels and insulin, which also influences a variety of other body functions through neurological mechanisms.69 Chambers et al. showed that sweet taste in the mouth affects muscle function as measured by both exercise performance and brain activity.71 The tests were performed on athletes with a sweet carbohydrate solution used in the mouth only – participants tasted then spit the solution out. They used both a 1-hour cycling test, which showed improved performance just by tasting, and functional magnetic resonance imaging (fMRI) to demonstrate that there are specific areas in the cortex associated with oral receptor stimulation. The authors state that the underlying mechanisms for this performance-enhancing effect do not appear to be metabolic but rather neurological, with afferent signals modifying motor output. That changes in motor function occur as a consequence of gustatory stimulation is evident from common examples such as with the administration of syrup of ipecac, which induces immediate vomiting. Other human studies have used fMRI to demonstrate that specific areas of the brain are stimulated with glucose, water and other nutritional substances. fMRI has shown neurons in specific taste areas of the cerebral cortex are associated with oral taste.72 Jeukendrup and Chambers believe that the immediate changes in muscle function due to sweet taste are associated with specialized receptors in the oral cavity that have not yet been identified.73
The search is growing to better understand the receptors for taste that effect muscle function.17 Goodheart first made the clinical observation in 1968 that taste stimulation affected muscle function, observations that are discussed elsewhere.14,16,26–28 As a result of Goodheart's original finding, many health-care professionals in various disciplines worldwide have since used this clinical tool (taste stimulation followed by the MMT) as an adjunct for both assessment and treatment.14,74
As stated previously, applied kinesiology procedures involve the assessment of changes in muscle function after a patient chews or sucks on food or nutrition.75 The method consists of stimulating the gustatory nerve receptors by having the patient chew or inhale the substance to be evaluated, and then manually testing a muscle for change. The muscle may appear stronger or weaker, depending upon the type of evaluation being made and the muscle's neurologic association with the substance stimulating the gustatory or olfactory receptors.
Controversy
The AK MMT system of biochemical evaluation is controversial. One reason for this is that there have been many modifications of Goodheart's original description. The applied kinesiologist uses the MMT to evaluate nutrition as an adjunct to standard laboratory, nutritional, and physical diagnostic methods. All factors of the examination should correlate, or something is being missed. Research sponsored by the International College of Applied Kinesiology points out that the use of the AK MMT to evaluate nutrition is not a viable approach in itself.76 Some researchers, rather than having participants stimulate the gustatory receptors with the substance being tested, have the individual hand-hold the substance or lay it on the belly; some even have the patient hold a bottle containing the substance to be tested. These modified systems are frequently taught to laypeople, who often do not have the anatomical knowledge necessary for accurate muscle testing nor a sufficient background in nutrition or general diagnostic ability.77–80
While our understandings of the neurological pathways that produce changes in muscle function remain incomplete, there is definite evidence in the literature of efferent response throughout the body resulting from stimulation of the gustatory and olfactory receptors.69–71,80–84 Some of the observed reactions to lingual stimulation have included, for example: (1) exercise performance and brain activity, (2) canine pancreatic secretion, and (3) altered plasma levels of estrone, follicle stimulating hormone, and luteinizing hormone.71,82,85 Despite the complexity of factors involved, this evaluation may become a useful adjunct to the standard methods used in determining a patient's nutritional and hormonal status and needs.15,16,24,86–96
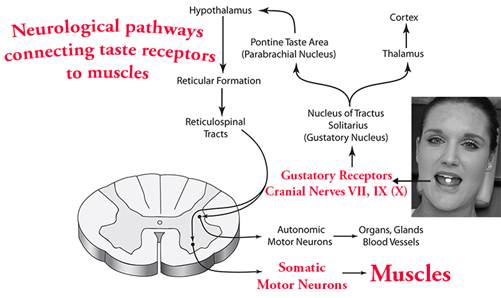
Figure 9: Proposed Pathways of Muscle Response to Gustatory Receptor Stimulation
AK MMT Examinations and Laboratory Tests: Concurrent Validity Review
Members of the International College of Applied Kinesiology have published outcomes research on adrenal gland dysfunctions since Goodheart first published an article on this in 1964.97 These have been presented in numerous clinical outcomes trials (case and case-series reports).14 The endocrine glands are of course controlled by the nervous system, and this may be why chiropractic has been helpful throughout its history for endocrine-related disorders.98
Deriving accurate and useful clinical prediction rules (CPR) for a variety of biochemical and neuromusculoskeletal conditions have been reported by biomedical and chiropractic researchers. This philosophical shift is in its professional infancy, but it is quite clear that it has an immediate impact on chiropractic and complementary and alternative medical practice, and it is likely that the professions will de-emphasize the application of nutritional or functional medical therapies based solely on biochemical theory and continue to develop and validate clinical prediction rules.
Figure 10
Schmitt and Leisman conducted a controlled clinical trial in an attempt to determine whether the AK MMT could identify individuals with specific hyperallergenic responses.16 Seventeen participants were found positive with AK MMT screening procedures indicating food hypersensitivity (allergy) reactions. Each participant showed muscle weakening (inhibition) reactions to oral provocative testing of 1 or 2 foods for a total of 21 positive food reactions. Blood drawn subsequently were both a radioallergosorbent test (RAST) and immune complex test for IgE and IgG against all 21 of the foods that tested positive with AK muscle screening procedures. These serum tests confirmed 19 of the 21 food allergies (90.5%) suspected from the AK screening procedures. This study represented a conceptual expansion of the standard neurological examination process for food allergies.
Lebowitz conducted an observational cohort study on 100 participants to evaluate whether oral nutrient testing of protein and starch together in a food-sensitive (hyperallergenic) group and in the non-food-sensitive control group produced differing findings on AK MMT.90 In the participants with no history of food sensitivities, a protein and starch combination produced weakening in 1 of the 50 participants. In the participants with a present or past history of food sensitivities, the protein and starch combination produced weakening in 46 of the 50 participants. 98% of the nonallergic group were unaffected by the protein and starch combination, whereas only 8% of the sensitive group were unaffected.
Moncayo and Moncayo are endocrinologists trained in musculoskeletal methods (AK) who have published a number of papers showing that the AK MMT can diagnose and properly guide treatment for patients with thyroid gland dysfunctions as detected by musculoskeletal examination findings and confirmed by blood testing.87,88
Jacobs and a research team from Northwestern College of Chiropractic conducted a multicenter clinical trial in 1984 involving 65 patients who were independently evaluated for thyroid dysfunction by AK and laboratory testing. 93 They found that therapy localization to the neurolymphatic and neurovascular reflexes for the teres minor muscle (associated in AK with the thyroid gland) correlated with standard clinical assessments of thyroid function. Each patient was rated on a scale of 1 (unquestionably hypothyroid) to 7 (unquestionably hyperthyroid). AK ratings correlated with clinical ratings (rs = .36, p < .002) and with laboratory ratings (rs = .32, p < .005). Correlation between clinical and laboratory diagnosis was .47, p < 0.000. Three AK therapy localizations had a significant correlation with the laboratory diagnosis (p < .05).
Page 1, 2, 3, 4 |
![]()
![]()






