|
Note: All figures also here, larger.
Page 1, 2, 3, 4
The human body is exposed to environmental toxins every day from a wide array of sources: particulate matter and diesel fumes in the air,1,2 heavy metals and other contaminants in the water,3,4 pesticide and herbicide residues found on foods,5,6 and even substances like bisphenol A (BPA) via contact with the skin.7 On a continuous basis, the body must work to eliminate toxic substances that are taken in. If intake exceeds removal, the toxins accumulate within the tissues and cells. These toxins tax our antioxidant systems, which must be upregulated in attempts to reduce cellular damage and death.8 But even with upregulation, the antioxidant protection system is often depleted by repeated insults and toxin exposure, and this depletion may contribute to disease processes.9 Chronic exposure to environmental toxins and toxic heavy metals is associated with the development of many types of cancer, respiratory disease, cardiovascular disease, diabetes, infertility, allergies, autoimmune disease, and many other conditions.10,11,12,13
Detoxification is the process by which the body eliminates substances that are both endogenous (such as hormones) and exogenous (such as medications, pollutants, metals, and other substances). In addition to cleaning up the diet and eliminating sources of toxicity, the use of chelating substances, antioxidant support, and therapeutic sweating are often the mainstays of detoxification protocols. However, these basic strategies, despite being crucial, lack consideration for other factors such as chronic infections, cholestasis, and enterohepatic recircu-lation of toxic substances that significantly impair the body's ability to detoxify. To comprehensively support detoxification, one must consider and address not only the glutathione system and its enzymes; liver, kidney, and gastrointestinal function; but also infections or dysbiosis, cholestasis, and the removal of toxins from circulation.
 Townsend Letter provides a platform for those examining and reporting on functional and integrative medicine. Please support these independent voices. Townsend Letter provides a platform for those examining and reporting on functional and integrative medicine. Please support these independent voices. |
Stages of Detoxification
The process of detoxification consists of three phases, although many people are only familiar with the first two of these. Phase I reactions involve the oxidation, reduction and hydrolysis of substances via enzymes from the cytochrome P450 (CYP450) family.14 It is Phase I metabolism that converts many drugs into their active compounds, and converts some chemicals into more toxic metabolites. Phase II metabolism involves the conjugation of toxins, creating larger, inactive, water-soluble molecules. Phase II reactions include sulfation, glucuronidation, and glutathione conjugation (see Figure 1).15
Figure 1: In a healthy state, toxins are processed and removed from the cells and organs via enzymes and transporter proteins, and leave the body primarily via the skin, urine, and feces.
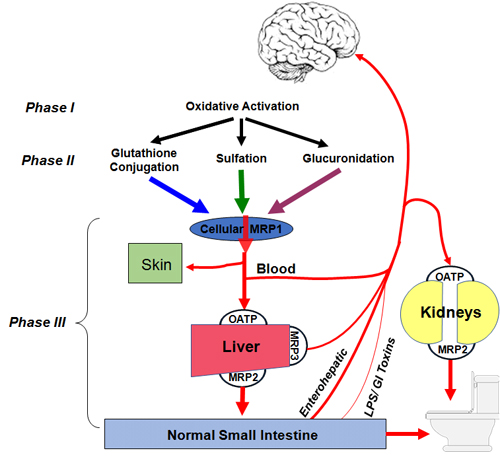
Phase III is often neglected in discussions of detoxification. However, it is critical. Phase III involves the process of transport and elimination of toxic substances through cellular membranes. The primary proteins that play a role in Phase III are multidrug resistance protein (MRP) 1, 2, 3, and 4, organic anion transport proteins (OATP), and P-glycoprotein (P-gp).16 These proteins also regulate the movement of molecules through barrier tissues, such as the blood-brain barrier.17
 The work horses for detoxification are 1) MRP1, the transmembrane transporter serving most cells in the body for exporting toxins to circulation, 2) OATP, the basolateral membrane transporter which moves toxin conjugates from the blood into the hepatocytes or renal tubule epithelial cells, and 3) MRP2, the apical transporter that moves toxin conjugates (and some bile salts) into the bile canaliculus or renal proximal tubule lumen. MRP3 and MRP4 are basolateral transporters that move toxin conjugates and bile salts from hepatocytes into the blood. All of the enzymes and transporters required for detoxification are present at a basal level, but many have increased expression in a coordinated fashion when stimulated by drug or toxin exposure.18,19 The work horses for detoxification are 1) MRP1, the transmembrane transporter serving most cells in the body for exporting toxins to circulation, 2) OATP, the basolateral membrane transporter which moves toxin conjugates from the blood into the hepatocytes or renal tubule epithelial cells, and 3) MRP2, the apical transporter that moves toxin conjugates (and some bile salts) into the bile canaliculus or renal proximal tubule lumen. MRP3 and MRP4 are basolateral transporters that move toxin conjugates and bile salts from hepatocytes into the blood. All of the enzymes and transporters required for detoxification are present at a basal level, but many have increased expression in a coordinated fashion when stimulated by drug or toxin exposure.18,19
Although the process of detoxification occurs in every cell of the body, the liver, kidneys, and intestines are primary tissues in which higher levels of detoxification occur.20 Many are familiar with the importance of the liver and kidneys as organs of detoxification, yet neglect awareness of the role of the intestines, the mucosal lining of which expresses high levels of the proteins important for all phases of detoxification.21,22 When any of these systems are impaired, a backup in processing of toxins will occur, with a greater burden being placed on other organs.
Nrf2: The Cellular Detoxification On-Switch
Nrf2 (short for nuclear factor E2-related factor) is a cellular switch that orchestrates antioxidant, detoxification, and cellular defenses. Nrf2 is present in the cytosol of the cell (see Figure 2), and responds to oxidative stress by translocating to the nucleus and binding to the promoter region of genes that encode the transcription of critical components of detoxification known as the antioxidant response element (ARE).23 In addition to elevated levels of reactive oxygen species (ROS), the Nrf2/ARE pathway is activated by a reduced cellular antioxidant capacity, and by exposure to toxic substances like air pollution and heavy metals.24,25
Figure 2: Oxidative stress causes Nrf2 to dissociate from binding protein (Keap1) in the cytosol and translocate to the nucleus where it binds the promoter region (ARE), leading to transcription of detoxification enzymes and proteins. Various substances have been shown to have an inhibitory or inducing effect on the Nrf2/ARE pathway.
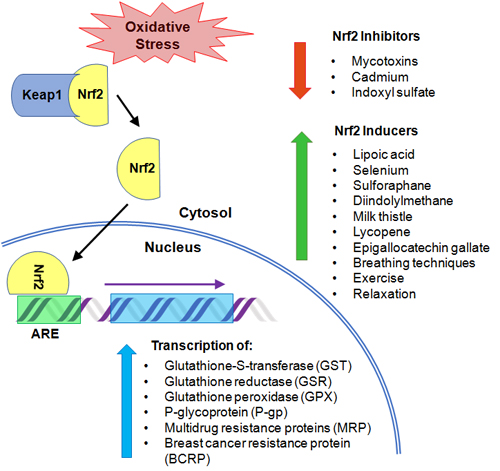
When activated, the Nrf2/ARE pathway can switch on over 200 genes that help the cell generate protective molecules (see Figure 2).26 This includes antioxidant elements, detoxification enzymes, and proteins required for glutathione synthesis and recycling such as glutathione S-transferase (GST), glutathione reductase (GSR), and glutathione peroxidase (GPX).27-30 Nrf2 also upregulates proteins responsible for Phase III detoxification (P-gp, BCRP, and MRP2) and the transfer of toxic substances out of the cell and central nervous system.
Factors that Impede Detoxification
Nrf2/ARE Pathway. Studies have shown that the ability to upregulate Nrf2 and its antioxidant-supporting action declines with age, which may be one reason the elderly are more susceptible to damage from environmental pollutants.31 Ochratoxin A, one of the most common mycotoxins found in foods and water-damaged houses, acts as a Nrf2 inhibitor (see Figure 2).32 Indoxyl sulfate, a uremic toxin that is increased in the blood with chronic kidney disease and exposure to toxic heavy metals such as cadmium, also acts as a Nrf2 inhibitor, further contributing to accelerated renal damage at the level of the tubules.33-35
Endotoxin. Lipopolysaccharide (LPS), also known as endotoxin, is associated with the outer membrane of gram-negative bacteria. Increased intestinal permeability, aka "leaky gut," allows for increased translocation of LPS from the gut into circulation. Damage to the intestinal barrier is common and can occur with infection, surgery, stress, intense exercise, celiac disease, food allergies, non-steroidal anti-inflammatory drugs (NSAIDs), and alcohol use (see Figure 3).36-38 Toxins, including heavy metals, pesticides, and herbicides such as glyphosate, also have been shown to lead to inflammation and/or increased permeability.39-43 With exposure to mercury, inflammation and increased intestinal permeability may occur due to oxidative stress and glutathione depletion.44
Figure 3: Gastrointestinal inflammation and increased intestinal permeability allow for endotoxin (LPS) to be released from bacteria in the gut into circulation. Endotoxin and related inflammatory cytokines block detoxification pathways by downregulating the detoxification enzymes and Phase III transporters, as well as contributing to cholestasis and kidney damage.
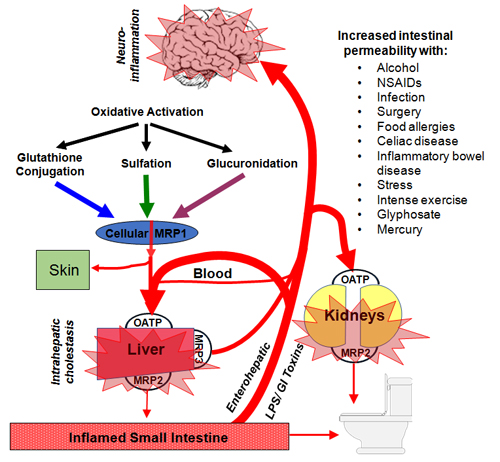
Page 1, 2, 3, 4
|
![]()
![]()
![]()
![]()









