|
Introduction
Primary myelofibrosis is classified in oncology under myoproliferative neoplasms. Myeloproliferative neo-plasms can demonstrate overproduction of one or more of the formed elements from the bone marrow and are said to be able to mimic one another.1
Myelofibrosis, along with poly-cythemia vera and essential thrombo-cythemia, comprises the BCR-ABL1-mutation negative members of a sub-group.1,2 Of this group, myelofibrosis has the shortest survival time, with a mean estimate of six years. Pharmaceutical therapy has not been shown to be curative or disease modifying. Only stem cell transplantation has potential for cure or to prolong survival.2
 Myelofibrosis is a genetic and metabolic condition (55-65% are accompanied by the gain-of-function JAK2 mutation), where fibrotic tissue begins to replace functional bone marrow.1 The initial action can be a crowding out of bone marrow with resulting pancytopenia, abnormally low white blood cells, red blood cells, and platelets. It is not a classic malignancy in the usual sense. Myelofibrosis is a genetic and metabolic condition (55-65% are accompanied by the gain-of-function JAK2 mutation), where fibrotic tissue begins to replace functional bone marrow.1 The initial action can be a crowding out of bone marrow with resulting pancytopenia, abnormally low white blood cells, red blood cells, and platelets. It is not a classic malignancy in the usual sense.
The term "fibrosis" refers to excessive deposition of extracellular matrix, which then becomes fibrosis or scar tissue. Fibrosis is considered the cause of most organ failure.3 It is driven by excessive transforming growth factor-beta and can involve genetic and epigenetic factors in the action pathway.4-6 The condition can be reversed, if production is decreased.3,7
When the described patient arrived with diagnosis of myelofibrosis, the initial thought was to treat this like a fibrosis problem because of the known lack of success from other therapeutic concepts. At 83 years old, she would not be considered for stem cell transplantation. How control of myelofibrosis was apparently accomplished, with partial resolution of pancytopenia and complete elimination of the projected weekly transfusions for maintenance, is described and discussed below.
Significant History from Medical Reports Prior to Consultation
June 2013: Atypical lymphocytosis "consistent with chronic lymphocytic leukemia" (CLL). Further results showed deletion at 13q and no deletion at 17p. "13q gives a more favorable prognosis for CLL."
September 2016: Bone marrow biopsy comments: Chronic lymphocytic leukemia (10% involvement); JAK2 mutation positive, marked reticulin fibrosis, consistent with myelo-proliferative neoplasm, such as primary myelofibrosis.
October 2016: Diagnosis of primary myelofibrosis with transfusion dependent anemia, thrombocytopenia, and leukopenia.
Consultation History
Visit 1 (10-13-16): Female, 83 years old with diagnosis (Dx) of CLL six years ago, with present Dx of primary myelofibrosis for three weeks. Requires RBC transfusion almost weekly. This is delivered by self-demand when hemoglobin tests low. The patient had been instructed how to recognize symptoms of low hemoglobin and would then report in for CBC and receive transfusion. Record of complete blood count varied widely because of maintenance by transfusion.
The patient had physical and lab signs of intestinal malabsorption and was instructed in gluten avoidance without lab diagnosis. Testing for gluten intolerance was not performed, as from the nature of the diagnosis and the frequent transfusions, a reliable result seemed unlikely. Testing was arranged for transforming growth factor-beta (TGF-beta) and prescription given for metformin-ER, 500 mg twice daily, and quercetin, 1000 mg twice daily.
Visit 2 (10-20-16): Astaxanthin, 12 mg twice daily, was added. Highly absorbed quercetin (as a "caged" molecule) was obtained from Tesseract Medical and provided after the visit (1/4 teaspoon, about 600 mg, containing about 105 mg quercetin).
Visit 3 (12-8-16): Patient showed the results of spontaneous bruising and bleeding under the skin, a likely outcome of her platelet level of 70. Vitamin K2 (15 mg daily as MK4) and berberine (500 mg twice daily) were added. After the addition of ¼ teaspoon daily of the "caged" quercetin to the treatment regimen, the patient went 19 days without requiring transfusion, more than twice as long as previously. Caged quercetin was now increased to twice daily.
Visit 4 (1-5-17): Patient is now requiring only one transfusion per three to four weeks. Continuing on a program of regular quercetin (1000 mg twice daily), ¼ teaspoon caged quercetin twice daily, metformin-ER 500 mg, and astaxanthin. (Miscommunication resulted in TGF-beta not being tested until after the lowering agents were in place, and it was not elevated.)
Visit 5 (2-15-17): Patient has had some degree of diarrhea for a while. (A full stool culture was ordered and showed a 4+ growth of Klebsiella pneumoniae. Antibiotic treatment resolved the diarrhea.) Vitamin K2 was increased to 15 mg twice daily. Last transfusion was five weeks ago.
Visit 6 (3-13-17): No transfusion has been required since January. (This status has continued through June 2017, over five months.) The patient furnished a copy of her supplement list that included metformin-ER (500 mg twice daily), quercetin (1000 mg twice daily), Tesseract quercetin (1/4 teaspoon, about 600 mg, containing about 105 mg quercetin twice daily), berberine (500 mg twice daily), vitamin K2 (MK4, 15 mg twice daily) and a number of nutritional supplements used before treatment began for myelofibrosis. Quotation from oncologist report of 3-17-17: "Clear benefit from alternative therapy provided by Dr. Lamson at the Tahoma Clinic with transfusion independence." See Figure 1 for the compete blood count history. Transfusion dates after the first consultation were as follows:
- 10-12-16,
- 10-21-16 (nine-day interval),
- 11-19-16 (29-day interval),
- 12-9-16 (20-day interval), and
- 1-11-17 (26-day interval and last transfusion).
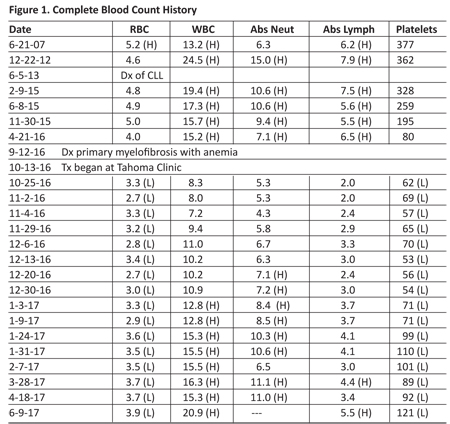
From the series of blood counts, the erythrocyte and platelet counts are stabilized and increasing with the present program, but the leukocyte level has increased into the abnormal range, both granulocytes and lymphocytes. A shift back toward the previous leukemia seems illustrated. Further, the shift has been rapid, and it is not yet known whether the leukocyte level will arrest near the previous high level and progress in the usual indolent CLL fashion or if this condition has become more aggressive.
Consultation with the medical oncologist will be obtained. One obvious approach, tapering the doses of the agents employed, could determine if a more favorable balance of erythrocytes and leukocytes is possible.
 Discussion Discussion
Fibrosis is a "common pathway to organ injury and failure."8 It seems chiefly driven by TGF-beta (transforming growth factor-beta).9 Excessive TGF-beta results in deposition of more extracellular matrix, which can become fibrotic tissue. TGF-beta normally limits cell production, but changes in epigenetic or genetic factors can remove the limitation and result in over-production of affected cells and further increase TGF-beta.10 Fibrosis is a reversible phenomenon and lowering TGF-beta can decrease it.4 There are many publications reporting on the decrease of fibrosis in kidney,11 lung,12 liver,13 etc. Searches of PubMed revealed at least 20 natural agents reported to do this. Unfortunately, there are no comparisons on degree of effectiveness.
On the basis of these findings, several agents were applied for the reasons described. Metformin has several anti-malignant actions, including in the hematopoietic area14-17 and can attenuate organ fibrosis.18 Astaxanthin can quench hydroxyl radical and possibly slow further DNA mutation.19 Quercetin has many anti-cancer mechanisms and is known to lower TGF-beta and reduce fibrosis.20-22 Further quercetin can inhibit the JAK/STAT cascade of inflammation and cell proliferation.23 Berberine contributes to lowering the mTOR pathway implicated in myelofibrosis.24,25 The vitamin K2 (MK4) was added because of spontaneous bleeding from low platelets and the reported benefit to myelodysplastic syndromes and leukemias.26
A search of PubMed indicates that this may be the first report illustrating control of myelofibrosis with refractory anemia (other than stem cell transplantation) and by mostly non-prescription agents. Questions that remain are whether this program will continue successful over a long period, whether it will apply to other patients, whether it will extend lifespan, and whether it acts for the presumed reasons. (There are pathways that encourage fibrosis other than TGF-beta as well as other pathways operated on by the agents employed.) Further, it should be mentioned that serum TGF-beta is not a reliable indicator of cellular TGF-beta (p. 959).27
Acknowledgement
Thanks to Jileen and Richard Russell's Smiling Dog Foundation and the Russell Family Foundation for support of this work.
References .pdf
 Davis W. Lamson, MS, ND, practices at Tahoma Clinic in Tukwila, Washington with chief interests in autoimmunity and cancer. He has published research and reviews on hepatitis C, controlling MRSA, stimulating immune function, emphysema, autism, diabetes, gastroesophageal reflux, kidney failure, autoimmunity, and various cancer-related topics. Davis W. Lamson, MS, ND, practices at Tahoma Clinic in Tukwila, Washington with chief interests in autoimmunity and cancer. He has published research and reviews on hepatitis C, controlling MRSA, stimulating immune function, emphysema, autism, diabetes, gastroesophageal reflux, kidney failure, autoimmunity, and various cancer-related topics.
Dr. Lamson was adjunct faculty and coordinator of oncology education for 17 years at the Medical School of Bastyr University and supervised ND medical students in a hospital oncology setting.
Dr. Lamson received the 2004 Bastyr University Distinguished Alumnus Award and the 2005 President's Award of the Oncology Association of Naturopathic Physicians on its founding. In 2015, he received the Lifetime Achievement Award of that association.
|
![]()
![]()
![]()
![]()









 Davis W. Lamson, MS, ND, practices at Tahoma Clinic in Tukwila, Washington with chief interests in autoimmunity and cancer. He has published research and reviews on hepatitis C, controlling MRSA, stimulating immune function, emphysema, autism, diabetes, gastroesophageal reflux, kidney failure, autoimmunity, and various cancer-related topics.
Davis W. Lamson, MS, ND, practices at Tahoma Clinic in Tukwila, Washington with chief interests in autoimmunity and cancer. He has published research and reviews on hepatitis C, controlling MRSA, stimulating immune function, emphysema, autism, diabetes, gastroesophageal reflux, kidney failure, autoimmunity, and various cancer-related topics.