Online publication only
Abstract
Objective: To obtain and examine MedWatch reports of cases of cognitive impairment associated with Lipitor (atorvastatin).
Methods: FDA database MedWatch reports of atorvastatin-associated adverse events were searched for terms that included the word amnesia. This search revealed reports listed as transient amnesia, transient global amnesia, wandering amnesia, anterograde amnesia, dissociative amnesia, and retrograde amnesia. No reports were uncovered using the terms memory loss, memory disturbance, or memory disruption; yet memory impairment revealed multiple reports. Searches were directed at only serious cognitive events. Minor events such as forgetfulness or confusion were not sought, and it is possible that we missed an occasional serious event listed under a mild symptom. The well-known Naranjo ADR Probability Scale was applied to 50 randomly selected case reports of Lipitor-associated cognitive dysfunction.
Results: Six hundred and sixty-two MedWatch reports were received of atorvastatin-associated cognitive impairments. Of these, 399 were cases of amnesia, and 263 were cases of memory impairment. The number of reports per year increased from 1997 through 2006. Random analysis of individual MedWatch reports demonstrated that most were definitely or probably caused by atorvastatin. The average atorvastatin dosage of cases in 1997–2001 was 15 mg/day, whereas the average dosage in 2006 was 22 mg/day. Earlier research suggests that the number of MedWatch reports for statin-linked adverse events greatly underestimates the scope of the problem. Other research suggests that statin drugs may cause subclinical yet important cognitive impairments in all patients receiving statins.
Conclusion: The findings of the present study, coupled with earlier research, demonstrate the urgent need for further research regarding the frequency and severity of cognitive impairments in patients receiving statin drugs.
Introduction
In 2004, the family doctor of one of the authors (DG) reported that he had contacted the manufacturer of atorvastatin to request information on atorvastatin-associated memory impairment. In response to the request, the doctor received results of the prerelease clinical evaluation phase of atorvastatin.1 Knowing that the data would be of interest to doctors involved in studying statin side effects, he shared the information with the author.
The document showed that, overall, 2502 volunteer patients with varying types of hyperlipidemia tolerated atorvastatin well at dosages up to 80 mg. Table 1, "Changes in Memory and Cognition," provided information on these events in study subjects.
Amnesia was defined as memory loss or increased memory loss; impaired, worsening, or lapses of memory; forgetfulness; short‑term memory loss; or decreased memory capacity. "Thinking abnormal" was defined as difficulty concentrating; abnormal, slow, or difficulty thinking; cognitive disturbance; decreased or slowed mental activity/function; impaired intellect, judgment or mentation; or irrational thinking.
Table 1: Results of Cognitive Impairments during Prerelease Clinical Trials
Adverse event Atorvastatin Other Statins
(N = 2502) (N = 742)
Amnesia 7 (0.3%) 2 (0.3%)
Abnormal Thinking 4 (0.2%) 0 (0.0%)
Overall, 11 cases of severe cognitive disturbance were identified among the 2502 patients receiving atorvastatin during the clinical evaluation phase. The rate of cognitive disturbance per 1000 subjects receiving atorvastatin was approximately 4.5. This finding suggests that among the millions of patients who take atorvastatin daily, 4500 cases of cognitive impairment would be expected per 1 million users of the drug.
In 2001, King and colleagues described two patients who presented with cognitive impairment.2,3 The first patient was a 67‑year-old Caucasian woman with hypertension, dyslipidemia, hypothyroidism, and diabetes, who presented with changes in behavioral characterized by mood alterations, lack of interest in routine activities, diminished short‑term memory (demonstrated on mental status examination), and social impairment.
Two months prior to this visit, atorvastatin 10 mg/day was increased to 20 mg/day. The patient had been previously controlled on atorvastatin 10 mg/day without experiencing any adverse events for one year. Atorvastatin was discontinued, but no changes were made to her other concurrent medications, which included levothyroxine, hormone replacement therapy, glyburide, and metoprolol. After discontinuation of atorvastatin, the patient reported dramatic improvement in mood, memory, and motivation. Repeat mental status examination also demonstrated marked improvement in short‑term memory. At six months postdiscontinuation, the patient had experienced no additional impairment.
The second patient was a 68‑year-old Caucasian woman with hypertension who was being treated long‑term with lisinopril, estradiol, and atenolol.3 Her initial evaluation revealed uncontrolled hypertension, hyperlipidemia, and an intact memory and judgment and insight. As a result, hydroclothiazide and atorvastatin 10 mg/day were added to her current drug regimen. Approximately nine months after this initial visit, the patient's daughter reported noticeable memory impairment, cognitive decline, and behavioral changes. The patient was forgetting scheduled routine social events and appointments and neglecting her longstanding exercise program. The patient discontinued atorvastatin on her own, and cognitive improvement was reported in one week.
One month after resolution of symptoms, the patient was rechallenged with atorvastatin; the cognitive impairment returned three weeks later. Atorvastatin was again discontinued; and one month later, the patient reported improvement in memory. Mental status examination demonstrated a return to baseline. Simvastatin 20 mg/day was initiated, and seven weeks later, the patient and her daughter reported a return of the memory impairment and cognitive decline. Three weeks after discontinuing simvastatin, these symptoms resolved.
In 2002, Wagstaff and others from Duke University did a MedWatch survey of cognitive dysfunction associated with the use of statins.4 Only cases in which the statin was considered the primary suspect in causing mental status change were included. From November 1997 through 2002, MedWatch received a total of 60 reports of statin‑associated cognitive adverse events, with 23 involving atorvastatin, 36 involving simvastatin, and one involving pravastatin. The mean daily dose reported for atorvastatin was 25 mg. Analysis of the reports revealed that 17 patients experienced short‑term memory loss, six experienced amnesia, and 37 had unspecified memory loss.
For the 30 patients with documented time to onset of memory loss after the start of statin therapy, median time was 60 days. Approximately 50% of these patients experienced memory impairment within the first two months. In addition, of the 33 patients (16 taking atorvastatin and 17 taking simvastatin) who withdrew from statin treatment, memory loss resolved or improved in 14 patients and no improvement was noted in 11 patients, whereas 8 patients indicated unknown cognitive function after statin withdrawal. Rechallenge with atorvastatin (n = 3) and simvastatin (n = 1) resulted in recurrence of symptoms.
The first time DG was given atorvastatin was during his annual physical. He experienced a six‑hour episode of transient global amnesia.5 When he suggested, on the basis of his 23 years as a family doctor, that perhaps his new medicine might be the cause of the amnesia, the neurologist disagreed, as did all the other specialists he saw subsequently. Nearly convinced that he was wrong to attribute his amnesic episode to atorvastatin, during his next physical one year later, he agreed to restart the statin at one‑half the previous dose. After about two months on atorvastatin, he had a second, more severe attack of transient global amnesia. He was suddenly 13 years old, and his memory of his adult life was abolished. The experience was terrifying. When his wife tried to assist him, he ran away from the stranger. The episode lasted 12 hours, at which time full cognitive function returned.
Methods
We examined the MedWatch data from November 1997 through January 2007 for spontaneous adverse events of cognitive impairment associated with the use of atorvastatin. Atorvastatin was chosen because of its large market share and because of the relatively large number of atorvastatin-associated cognitive complaints reported to us, compared with those associated with the use of other statins. The People's Pharmacy syndicated newspaper column, reporting this in 2000, had focused just on atorvastatin-associated amnesia events. The resulting publicity resulted in a flood of reports of statin events to author DG's website (www.spacedoc.net) and served as the basis for his repository. His personal repository now contains more than 6500 of these reports and consists of all side effect events from all statins.
The FDA, as well as pharmaceutical companies, has dedicated proprietary software for analyzing and conducting searches of adverse event reports, and the dictionary used to code MedWatch adverse event terms is also proprietary; neither the software nor the dictionary was available to us. Our review of MedWatch data was conducted on a personal computer using word search. The following terms were identified as appropriate: Searching for amnesia uncovered reports under this term, but also reports listed as transient amnesia, transient global amnesia, wandering amnesia, anterograde amnesia, dissociative amnesia and retrograde amnesia. No reports were uncovered using the terms memory loss, memory disturbance, or memory disruption, yet memory impairment uncovered multiple reports. Although our search was thorough, our objective was to identify significant cognitive problems. We did not seek to identify minor cognitive events such as forgetfulness or confusion. In excluding minor events, it is possible that we unintentionally excluded some major ones. Therefore, our result for significant cognitive impairments may be an underestimate.
Although each MedWatch report contained age, sex, date, and statin dose, experience soon revealed that this information was too inconsistent to be of value. In nearly half of the reports, one or more of these were absent; and even the dates, which one might think would be reliable, proved questionable, when on many occasions, the same date would appear consecutively on dozens of reports, as if a technician had just returned from a long absence and was hurrying through the backlog. As a result, this study is primarily descriptive. We have included several case reports typical of the hundreds reported to MedWatch as examples.
For application of the Naranjo ADR (adverse drug reaction) Probability Scale, 50 case reports were randomly selected from our repository and reviewed one by one for classification.6 Certain factors having to do with the almost complete lack of awareness within the medical community of cognitive effects with statin use made application of this scale challenging.
Results
The results listed in Table 2 were derived from the MedWatch database containing reports of cognitive impairments associated with the use of atorvastatin.
Table 2: MedWatch Reports for Atorvastatin-Linked Cognitive Impairments
Amnesia Memory Impairment
1997 1 0
1998 12 2
1999 14 9
2000 26 1
2001 46 32
2002 20 55
2003 20 29
2004 65 35
2005 86 41
2006 91 58
Jan 2007 18 0
Total 399 263
A glance at these figures will show that since 2004, there has been a substantial increase in reported events per year. This is particularly true for 2007, where the January reports, extrapolated over the full year, promised to yield over 180 amnesia reports. The numbers become of much greater significance when one realizes that they are reported in a climate in which neither the patient nor the doctor truly comprehends the causative relationship of statin to cognitive dysfunction. The average doctor today is startled when apprised of the evidence, and patients are even less likely to make the association of cognition disturbances with statins.
The dosage of atorvastatin was specified in 109 of the 399 amnesia reports. The mean atorvastatin dosage used in the first 50 MedWatch cases (1997 to 2001) was 15 mg/day. In the last 50 MedWatch cases (2006), the dosage was 22 mg/day. When one considers that, in clinical practice, atorvastatin is prescribed at doses ranging from 10 to 80 mg/day, these mean doses are relatively low.
Concomitant disorders frequently listed in the MedWatch reports included hypertension, hypercholesterolemia, history of stroke, history of myocardial infarction or other heart problems, and diabetes types 1 and 2. Concomitant drugs included thyroid replacement, hormone replacement, beta blockers, angiotensin-converting enzyme inhibitors, calcium channel blockers, NSAIDS (nonsteroidal anti-inflammatory drugs), and steroids.
Many of the cognitive reports display a close association of the cognitive impairment with the beginning of atorvastatin treatment or following a recent dosage increase. Also notable is that people having transient global amnesia can appear remarkably functional, retaining full capacity for normal everyday activities such as walking and driving an automobile. They can talk normally, but none of this is relevant, for they are unaware of anything they are told. Many reports tell of lack of physician awareness with tendency to dismiss any possibility of statin causation. Although transient global amnesia is often the first evidence, many victims will have demonstrated short-term memory deficits as well. Additionally, the cognitive dysfunction may be so subtle as to be dismissed for years as just "age." The following four examples reflect these.
Case 1: I am a pediatric nurse practitioner who just had a very scary transient global amnesia (TGA) experience with my 55-year-old mother. She is in good health, works out at the gym four to five times a week, and besides Lipitor and Lotensin for blood pressure, is on no other medications. We just got back from vacation, and she had an acute episode of TGA. It lasted about four hours, and she has no recollection of that time. I was a little nervous because we thought she was having a stroke. The strange part was that she had no other deficits during the episodes and all tests were negative (CT, MRI/MRA, carotid Doppler, echo, stress test, lab work). We happened on an article in Family Circle magazine about TGA and Lipitor. Her Lipitor had been increased in the last few months to 40 mg. I then did a web search from the hospital room and found all of this info on TGA and Lipitor. It made us feel better, yet when my father brought it to the attention of the neurologist and cardiologist there, they chuckled and blew it off while discharging her still on 40 mg of Lipitor. We are just arriving home and starting follow-up and just wanted to share this experience.
Case 2: I am a physician and was just diagnosed with TGA after a few scary days in the hospital. All of my tests were normal, but I do take Lipitor. My son, who is also a physician, told me that he noticed a subtle difference in my short-term memory over the past year. The neurologist friend said he had heard about this reaction to statins. My partner had heard about this also. The other physicians I have spoken with, who are trusted friends and respected colleagues, do not give credence to your hypothesis. I, however, want to find the possible reason for this most traumatic and disturbing incident in my life.
Case 3: My husband has been on Lipitor for several years, and I/we have noticed that more and more his memory and focus have been impaired. We are told that there is no such evidence that Lipitor could cause this. I have watched my husband change from a Harvard Business School graduate, who could accomplish more in four hours than most could in four days, to someone who has already had a TGA attack and, in the two years since, has become more forgetful, is unable to complete tasks, loses track of time – just about everything. I was wondering if you knew of any doctors in our area who specialize in this. We would be willing to travel to another state to see a specialist. It has been going on too long. We know there is a problem and desperately need help. Thank you.
Case 4: Just a note to let you know of an episode that my brother had recently that we feel was probably caused by Lipitor. After dinner last week with my uncle and cousin, my brother went to get the car at a lot a block away. After getting the car, he made a wrong turn and then got confused as to where he was and how to get back to where we were. (He knows this area of town well and is a teetotaler). I talked with him via cell phone, and he told me the names of the streets he was passing. I said he was going the wrong way and needed to turn around. He continued to head north, and we were south. I finally persuaded him to get off the expressway and pull over on the side of the street, whereupon I called the local police, told them approximately where he was, and hoped they would find him (I thought he was having a TIA, in part because his speech was somewhat garbled and because of the disorientation). After five minutes and before the police could find him, he hit the road again and started driving to a nearby hospital but was headed in the wrong direction. The police finally intercepted him about a mile from the hospital, where he was taken and given a battery of tests, all of which were negative. Upon his release, about 18 hours later, he was told to get an EEG and an MRI of the brain (negative and negative). In the meantime, I have learned much more of this from the Internet. My brother has been on Lipitor for about a year, and a few weeks ago, his dosage was increased from 10 to 20 mg. Thanks for your insights.
With respect to application of the Naranjo ADR Probability Scale to such reports to better grade ADR reports as definite, probable, or unlikely, we have the obstacle of almost complete lack of awareness by the medical community that statin drugs can do this. If we can now dismiss this obstacle, we can state that most of the 50 reports could be placed in the "definite" category. Although most of the time, cognitive dysfunction takes place within the first few months or after dosage increase, in some cases, years pass before side effects are manifest. Because of this, a few of the reports must be placed in the "probable" category. Most cases had immediate improvement in amnesia episodes with withdrawal of the drug; however, in a very small number, one or more amnesia episodes occurred up to six months after the drug was stopped. With respect to short-term memory loss, most progressively recovered fully, but a very few still have serious decrement four years from the original problem In this group of 50, only two allowed rechallenge. One (DG) rechallenged with atorvastatin at half the previous dose; the result was strongly positive, with a much more severe episode of amnesia. One other allowed rechallenge with another statin to find recurrence of the previously noted cognitive loss almost immediately.

Discussion
Glial Cell Cholesterol and Cognition
Pfreiger's article on the importance of cholesterol for normal brain function is particularly relevant here.7 The brain's synapses for memory formation cannot function without sufficient cholesterol, and since the LDL cholesterol molecule is much too large to pass the blood-brain barrier, nature devised an alternative means of supplying the brain with necessary cholesterol. Pfrieger found that the housekeeping cells of the brain, known as glial cells, had taken over the role of cholesterol synthesis. It seems likely that the inhibitory effect of statin drugs on cholesterol synthesis extends to our glial cells, and this might account for the many varieties of cognitive dysfunction reported. This might also explain why the more lipophilic statins seem to engender cognitive impairments more often than hydrophilic ones. Complaints of amnesia, forgetfulness, confusion, disorientation, increased senility symptoms, and short-term memory loss may all be related to this mechanism.
Mevalonate Pathway and Dolichol Inhibition
All statins, regardless of brand, are reductase inhibitors. As such, they block the mevalonate pathway common to the synthesis of CoQ10, dolichols, the operation of normal phosphorylation channels, and selenoprotein synthesis. The relationship of dolichol to emotion, behavior, and cognition is due to its role in glycoprotein synthesis (Figure 1).
Figure 1: Mevalonate Pathway
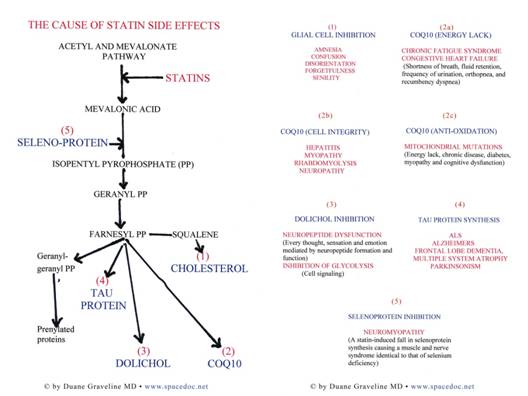
The reason for statin drug side effects are better appreciated by using this figure of the mevalonate pathway, which one might see in any standard biochemistry book. All statins are reductase inhibitors and therefore exert their effect at the very beginning of the mevalonate pathway. This pathway is shared by several other vital functions, including CoQ10 and dolichols. To inhibit the reductase step in an effort to reduce cholesterol synthesis is to "gird" the entire mevalonate tree and inhibit all the elements sharing this path. All the side effects of statin use can be predicted by a simple glance at this figure.
Glycoprotein Synthesis
Glycoprotein synthesis, the attachment of sugars to a growing peptide strand, is vital to neuropeptide formation, cell identification, cell messaging, and immunodefense.8 The entire process of sugar attachment to protein, taking place in the endothelial reticulum and Golgi apparatus of every cell, is orchestrated by dolichols. Dolichols govern the direction of folding and degree, thereby determining the ultimate molecular structure. Dolichols, like CoQ10, are severely depleted by statins. The consequences of dolichol insufficiency will be felt widely throughout the body. Because of the natural interplay and close relationship between emotion and memory, a possible effect of dolichol insufficiency on cognition is strongly suspected.
Statins and Selenoproteins
Another mechanism that may enter into statin-associated cognitive dysfunction is the well‑known statin inhibition of selenoprotein synthesis, a field of research recently promoted by the work of Mooseman and Behl.9 These researchers have demonstrated that selenium and selenoprotein deficiency due to the inhibitory effect of statins contributes not only to myopathy in general but also to cognitive side effects and others.
Research on this mechanism of statin side effects has only just begun, but the list of potential areas of investigation involving selenoprotein and the consequences of statin inhibition is growing rapidly. Selenoprotein dysfunction has been linked to multi‑minicore disease, a congenital myopathy that is characterized histologically by minicore lesions (focal areas of myofibrillar disorganization) and loss of mitochondrial function. In addition, selenium deficiency can cause a painful myopathy with thinned myofibrils, vacuolization without fibrosis, and mitochondrial abnormalities Their comprehensive review article is required reading for anyone interested in statin side effect mechanisms. Only a few years ago, the effect of statins on selenoprotein metabolism was unknown, yet now these effects are so broad they may encompass the full breadth of side effects currently reported with statin use.
Mitochondrial Mutations
In addition to possible statin-induced effects from altered selenoprotein metabolism, mitochondrial variations may result from free radical buildup as a consequence of statin drug interference with the synthesis of not only CoQ10 (see Figure 2) but also glutathione and other antioxidant enzymes.10,11 These powerful antioxidants are reduced to minimal levels by statins, which leads to the accumulation of free radicals in the highly oxidative environment of our mitochondria. This in turn produces an escalation in the rate of mitochondrial mutations. The recent report of Mootha and others is of immense importance in explaining drug-associated side effects.12 After introducing nearly 2500 drugs, many of which are FDA-approved, to their "mitochondrial toolkit" testing, these researchers immediately discerned new insights into basic mitochondrial function, which in turn revealed why some commonly used drugs have particular adverse effects. Mootha's team looked at the statin class of drugs wherein previous findings suggested that mitochondria were involved. They found that three out of the six statins (Fluvastatin, Lovastatin, and Simvastatin) interfered with mitochondria energy levels because of mutations and, when combined with the effects of certain blood pressure medications, were even worse. Research-oriented neurologists and rheumatologists now are beginning to suspect that some of their cases of myopathy, neuropathy, and even certain of our neurodegenerative diseases may be due to altered mitochondrial status from mutations related to statin exposure. Not only do statins deplete CoQ10, but through interference with selenoprotein production, they deplete the enzymes necessary for CoQ10 and glutathione regeneration, leaving mitochondria unprotected from the mutagenic effects of free radicals.
Incidence of Statin-Associated Cognitive Deficit
In a double‑blind, placebo-controlled trial, Muldoon et al. assessed cognitive function and psychological well‑being in 194 healthy adults.13 Subjects were 24 to 60 years old and had LDL cholesterol levels of 160 mg/dl or higher. Each subject was randomly assigned to receive 20 mg/day of lovastatin or placebo for six months. Serum lipid levels were measured throughout the study. At baseline and at completion of treatment, comprehensive neuropsychological tests were conducted for attention (digit vigilance, letter rotation, digit span, recurring words), psychomotor speed (grooved pegboard, maze, digit symbol), mental flexibility (strobe interference, trail making, digital vigilance, letter rotation), working memory (associated learning, digit span), and memory retrieval (controlled word association, and digit symbol recall, verbal recall, complex figure).
Psychological well‑being was assessed by daily diaries and subject interviews. At six‑month follow‑up, the placebo group had improved significantly in all five domains of cognitive function. The lovastatin group did poorly by comparison. Muldoon's interpretation was that 100% of statin users can expect a decrement in cognitive function. Three years later, Muldoon et al. repeated this study using simvastatin. The results were similar to the lovastatin study.
These results demonstrate that cognitive impairment can be found in all patients receiving statin medications if sufficiently sensitive testing is used. Such impairment may not be apparent. Our brains are not precise instruments, and substantial decrement can be present without being evident either to the patient or observers.
Muldoon's findings, coupled with our other findings, demonstrate an urgent need for studies to define the frequency and severity of cognitive impairments in patients receiving statin drugs. In the prerelease studies, severe cognitive impairments were seen at a rate of 4.5 per 1000 atorvastatin users. This finding suggests that 4500 cases will be seen per 1 million users of atorvastatin. Analysis of MedWatch reports of cognitive impairments linked to the use of atorvastatin demonstrates that many of these cases are definite or probable atorvastatin-induced events. Our collection of 662 MedWatch reports from 1997 through 2006 of atorvastatin-associated cognitive impairments is not large in relation to the widespread use of the drug. However, a recent study by Golomb et al. suggests that the number of MedWatch cases for statin drugs may grossly underestimate the extent of the problem because of physicians' failure to identify or report obvious cognitive impairments in patients receiving statins.14

Conclusions
- The 662 MedWatch reports of atorvastatin-associated cognitive impairment suggest a causal linkage between the drug and the reported events. Random analysis of the MedWatch reports demonstrated a high frequency of cases that were definite or probable, thereby adding weight to the possibility of a causal connection between atorvastatin and cognitive impairments.
- Accepted reporting rates to MedWatch of drug-related adverse events is 2.5 to 5%. Golomb et al. suggest it may be even lower with statin-associated adverse events. If 2.5% of atorvastatin-associated cognitive impairments are reported to MedWatch, then our 662 cases become 26,480 from 1997 through 2006. If 1% of cases are reported to MedWatch, then 66,200 cases of atorvastatin-associated cognitive impairments may have occurred.
- Statin impairment of glial cell synthesis of cholesterol is the most likely mechanism, but others must be considered.
- There is reasonable research evidence that 100% of statin users suffer some cognitive deficit that is not evident to them.

Notes
1. Joseph Tuazon, PharmD. Medical Information Manager, Pfizer U.S. Medical Information. NDA (New Drug Application) studies. Changes in Memory and Cognition with Tables 1&2. Pfizer Inc. 182 Tabor Road, Morris Plains, NJ 07950, 14 June 2006.
2. King DS et al. Cognitive impairment associated with simvastatin. Pharmacotherapy. 2001;21:37.
3. King DS et al. Cognitive impairment associated with atorvastatin and simvastatin. Pharmacotherapy. 2003;23(12):1663–1667.
4. Wagstaff L et al. Statin associated memory loss: analysis of 60 case reports and review of the literature. Pharmacotherapy. 2003;23(7):871–880.
5. Graveline DE. Lipitor, Thief of Memory. Self-published; 2003.
6. Cohen JS. Statin Drugs and Their Natural Alternatives. Chap. 7. New York: Square One Publishers; 2005.
7. Pfrieger F. Brain researcher discovers bright side of ill-famed molecule. Science. November 9, 2001.
8. King MW. Indiana University School of Medicine. Medical Biochemistry Page [website]. http://themedicalbiochemistrypage.org.
9. Mooseman B, Behl C. Selenoprotein synthesis and side effects of statins. Lancet. 2004;363:892–894.
10. Pregenzer JF, McKim JM Jr, Wilga PC. Anti-hypercholesterolemia drugs in the statin class reduce glutathione levels and increase caspase 3 activation in an in vitro cell model. Available at: http://www.ceetox.com/downloads/ceetox_sot_poster_statins.pdf.
11. Nordman T et al. Regeneration of the antioxidant ubiquinol by lipoamide dehydrogenase, thioredoxin reductase and glutathione reductase. Biofactors. 2003;18(1–4):45–50.
12. Mootha V et al. New chemical toolkit manipulates mitochondria, reveals insights into drug toxicity. Nat Bio. Epub February 24, 2008.
13. Muldoon MF et al. Effects of Lovastatin on cognitive function and psychological well being. Am J Med. 2000 May;108(7):538–546.
14. Golomb et al. Conceptual foundations of the UCSD Statin Study: A randomized controlled trial assessing the impact of statins on cognition, behavior, and biochemistry. Arch Int Med. 2004;164:153–162. Available at: http://econ.ucsd.edu/~mbacci/white/pub_files/hwcv-088.pdf.
|



![]()
![]()
![]()


