|
Page 1, 2
Chronic, nonhealing wounds are a significant issue. Impaired healing of often-horrific chronic wounds and ulcers affects over 7 million patients and over 1.75 million diabetic patients a year in the US. Approximately 29.1 million Americans (9.3% of the population) had diabetes in 2012. Their numbers will continue to rise. All diabetics suffer with impaired wound healing.1-3 Regardless of specialty, most physicians and practitioners will be faced with patients with wound-healing complications – often including diabetes – affecting the choice of modalities and protocols.
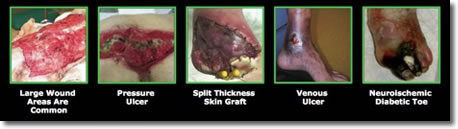
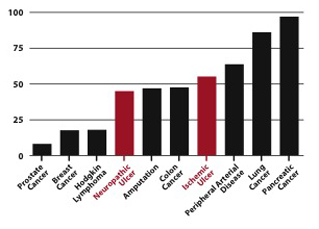
Because there is no effective treatment, a limb-related diabetes amputation is performed every 8 minutes in the US and every 20 seconds worldwide. Diabetic foot ulcers can have higher mortality rates than many cancers, including prostate and breast cancer, Hodgkin lymphoma, and colon cancer (Figure 1).4,5 Neuropathy and ischemia are the primary underlying risk factors for diabetic foot ulcers.6 Because the diabetic patient isn't aware of skin irritations, lack of sensation from neuropathy will often further aggravate the condition. Five-year mortality rates after new onset diabetic ulceration are between 43 and 55% – up to 74% for patients with lower-extremity amputation. Even with adequate arterial inflow, diabetic foot ulcers have only a 24% closure rate at 12 weeks and only a 31% closure rate at 20 weeks.7
Figure 1: Mortality rates
Nearly one-third of patients in hospital-based outpatient wound centers may not heal their wounds even though they are cared for over a long period of time.9 Arterial ulcers are often extremely painful. Their healing is often more difficult because of the additional issues caused by a compromised cardiovascular system. Patients with an arterial ulcer show a higher rate of recurrence and nearly twice as many amputations.6
Conservatively, according to 2007 data, costs for treatment and care of chronic nonhealing wounds of American patients exceeded $50 billion.9 Thirty-eight billion was linked to the treatment of foot ulcers – approximately one-third of the $116 billion in direct costs generated by the treatment of diabetes and its complications.6 As treatment duration lengthened, the cost of care significantly increased.5 Prevalence of diabetic foot ulcers will only increase in the future. There are no effective ingestible drugs to speed wound healing – moist wound care, bioengineered skin, negative pressure therapy (NPWT), growth factor enhancers, aspirin, and hyperbaric oxygen treatment (HBOT) may all be used with differing degrees of results.
Plant-Based Oils: 30 Days to Successful Patient Healing
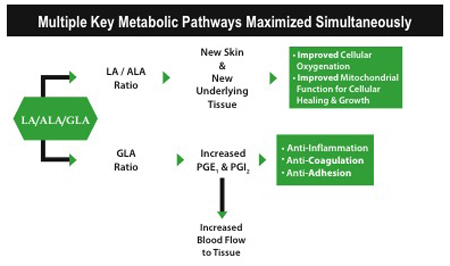
Three plant-derived components: Linoleic acid (LA), alpha-linolenic acid (ALA), and gamma-linolenic acid (GLA) – crucial compounds both directly utilized and metabolized to important eicosanoids – have been shown to be effective in treating complications of diabetes and, specifically, wound healing.10 Because of the skin's EFA composition, maximum skin/epithelial tissue healing occurs with formulations containing more metabolically active LA than ALA.
First and foremost is "sealing the wound." Skin (epithelial tissue) is composed almost exclusively of the EFA linoleic acid (LA). For rapid manufacture of new skin to seal the wound, ensuring adequate, metabolically active LA is crucial.10
Next, inflammation must be minimized or the wound/ulcer's surface skin will not heal expediently, nor will its underlying tissue. Inflammation pathways promote thrombosis (clogged arteries), impeding blood flow and wound healing.11 GLA supports maximization of PGE1 for decreasing thromboses impeding blood flow.
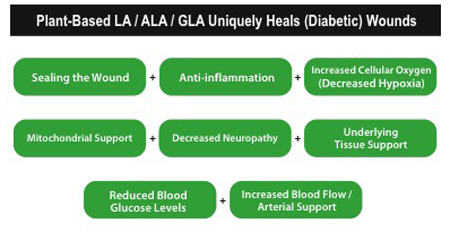
Increased cellular oxygenation/increased cellular (mitochondria) energy: Increased cellular oxygen accelerates wound healing and protects wounds from infection, but because of high oxygen consumption requirements, the environment of early wounds is quite hypoxic (oxygen deficient). Always accompanied by hypoxia, chronic wounds can have as little as 10% of the oxygen content of normal tissue.12 Via cardiolipin support, wound tissue can now obtain the required extra energy for repair, significantly accelerating healing.13-15
Accelerated underlying tissue repair: By optimizing cellular functionality with LA/ALA, all underlying tissue that is related to the wound/ulcer heals better because its cellular tissue membranes contains 25% to 33% LA/ALA.16
Reduced diabetic blood glucose levels: In part because of prolonged elevated blood glucose levels, damage to nerve function (neuropathy) occurs in more than 90% of diabetics. A calibrated LA/ALA formulation maximizes insulin-binding sensitivity, lowering elevated blood glucose levels. Patients taking LA lowered their blood sugars by an average of 15 points – very significant.17 In 2013, LA's effect in reducing diabetic blood glucose level was reconfirmed.18 A combination of LA and its metabolite GLA works synergistically in the cell membrane to reduce blood glucose and fortify the cellular fatty acids removed by elevated Lp-PLA2 in diabetics.19
Increased blood flow and arterial protection: Maximum blood flow is required for maximum wound healing. Decreased blood flow causes complications – from impaired oxygen transport (hypoxia) to impaired nutrient delivery required for expedient wound/ulcer healing. Diabetics are at a significantly increased risk of cardiovascular obstruction. Plant-based LA/ALA/GLA works synergistically to reverse existing cardiovascular disease (in particular, occlusions) in the diabetic patient.20,21 Plant-based oils support "natural blood thinning" for maximum arterial blood flow and optimize multiple protective cardiovascular pathways simultaneously.22,23 It is now known that metabolically active plant-based LA is effective in reversing heart disease, and that ALA is associated with less risk of a heart attack.24,25
 Clinical Success – Physician Case Studies with Peskin Protocol EFAs: Just 30 Days to Clinical Effectiveness in Healing Diabetic Ulcers and Underlying Pathophysiologic Disorders, Increasing Blood Flow, and Improving Surgical Outcomes Clinical Success – Physician Case Studies with Peskin Protocol EFAs: Just 30 Days to Clinical Effectiveness in Healing Diabetic Ulcers and Underlying Pathophysiologic Disorders, Increasing Blood Flow, and Improving Surgical Outcomes
October 22, 2015 – Case study: Nonhealing ulcer success – amputation prevented:
I just received a text last night from a patient that I prescribed the Peskin Protocol EFAs last month. He had severe type 1 diabetes with all of the vascular complications. He underwent a pancreatic and kidney transplant. He had a nonhealing ulcer on his right foot and was booked for amputation. He also has diabetic neuropathy. He texted me last night, after 5 weeks taking Peskin Protocol EFAs, stating: "There is a difference. I have less pain, walking better, and my foot is healing." Avoiding an amputation is a considerable feat! We have not only improved his life but saved the health system tens of thousands of dollars with just this one success.
March 27, 2015 – Case study: Improved blood flow (decreased occlusion) – amputation prevented:
I just saw an interesting patient who I've known for a while. She came to see me last month. The surgeons wanted to amputate her right leg due to arterial occlusion. She had a cardiac bypass and suffered daily angina attacks. I immediately prescribed the Peskin Protocol EFAs and saw her today. The angina is totally gone and the right leg is warm and pink! The Peskin Protocol EFAs will save her leg. Tremendous, in only 1 month!
Jeff Matheson, MD, pain specialist, Toronto, Canada
March 10, 2010 – Case study: Neuropathic patient unable to walk; can now walk:
A 16-year-old boy, Diabetic (Type 1) for 8 years presented with retinopathy, nephropathy, and neuropathy, HbA1c over 14%, unable to walk or put weight on both feet due to severe pain. He was on Narcotics. Placed on specialized vitamin and mineral formula (Treolife VM) and Peskin Protocol EFAs. 10 weeks later, his HbA1c dropped to 7.3% and he is able to walk on his feet without pain and discontinued his narcotics.
On his specialized vitamins, minerals, and EFA supplement, his HbA1c dropped to 6.6% 8 months later and to 6% 11 months after its institution.
Amid Habib, MD, pediatric endocrinologist specializing in diabetes Altamonte Springs, Florida
February 25, 2008 – Case study: Major surgery (wound) healing – improved patient outcomes:
In my practice as a plastic surgeon, I have found myself understanding that to obtain good post-operative results according to the intensity that varies from minor to major operations (the majority are very intense operations), the repair phlogistic [inflammation] resolution, edema and the scar tissue are all key factors to success. I must point out a new major factor that improved greatly my patients' surgical results after introducing Peskin Protocol EFAs plant-based oils from 15 days prior to 30 days after surgery. The level of tissue repair is what I look for especially in my practice and having the trial opportunity of five patients using Peskin's recommendations; I found in all five patients an enormously improved result with better recovery.
The Peskin Protocol EFAs do not cause excessive bleeding. In fact, it makes surgery easier and improves patient recovery. This improved recovery included:
1. faster healing
2. less inflammation
3. less scar tissue and
4. less pain to the patient
Dr. Andrea Roncarati, plastic/reconstructive surgeon Ferrara, Italy
Page 1, 2
|
![]()
![]()
![]()









 Clinical Success – Physician Case Studies with Peskin Protocol EFAs: Just 30 Days to Clinical Effectiveness in Healing Diabetic Ulcers and Underlying Pathophysiologic Disorders, Increasing Blood Flow, and Improving Surgical Outcomes
Clinical Success – Physician Case Studies with Peskin Protocol EFAs: Just 30 Days to Clinical Effectiveness in Healing Diabetic Ulcers and Underlying Pathophysiologic Disorders, Increasing Blood Flow, and Improving Surgical Outcomes